Sprained ankle
| Sprained ankle | |
 | |
|---|---|
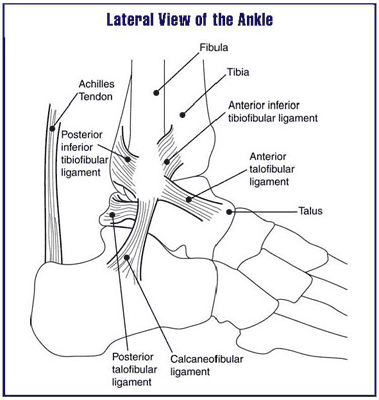
| Lateral view of the human ankle |
|
WikiDoc Resources for Sprained ankle |
|
Articles |
|---|
|
Most recent articles on Sprained ankle Most cited articles on Sprained ankle |
|
Media |
|
Powerpoint slides on Sprained ankle |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Sprained ankle at Clinical Trials.gov Trial results on Sprained ankle Clinical Trials on Sprained ankle at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Sprained ankle NICE Guidance on Sprained ankle
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Sprained ankle Discussion groups on Sprained ankle Patient Handouts on Sprained ankle Directions to Hospitals Treating Sprained ankle Risk calculators and risk factors for Sprained ankle
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Sprained ankle |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Javaria Anwer M.D.[2]
Synonyms and keywords: Ankle sprain; ankle injury; ankle ligament injury
Overview
A sprained ankle is a common medical condition where one or more of the ligaments of the ankle is/are stretched, partially or completely torn. Ankle sprains are more common among physically active individuals. The anterior talofibular ligament is one of the most commonly involved ligaments. Sprains to the lateral aspect of the ankle account for 85% of ankle sprains. Females are more commonly affected with an ankle sprain than males. The diagnosis of most ankle sprains is made in the light of history of acute ankle trauma and examination findings.
Classification
| Grading for functional loss of Ankle sprain | ||
| Grade | Degree of ligament damage | Symptoms and signs |
| Grade I | Mild stretching |
|
| Grade II | Incomplete tear |
|
| Grade III | Complete tear |
|
Pathophysiology
- The pathogenesis of ankle sprain is characterized by ankle movement beyond the elastic limits of its supporting structures causing acute ankle pathology.
- Lateral ankle sprain injury is usually caused by forefoot adduction, hindfoot inversion, and tibial external rotation with ankle in plantar flexion. Depending on the amount and direction of the force, one or more of the lateral ligaments can be involved.[2]
- The ATFL is the most commonly injured structure with the lowest load to failure when compared to the other lateral ligaments. The anterior tallofibular ligament (ATFL) is the most commonly injured ligament and is most susceptible to injury during ankle plantarflexion with the ankle's bony anatomy providing less stability. In this position, ATFL acts as a collateral ligament to the ankle. The ATFL prevents talar internal rotation, anterior translation and is a restraint to plantarflexion. The most common mechanism of injury to the ATFL is inversion injury where a plantarflexed ankle undergoes supination and adduction.[3]
- An ankle sprain can involve any of the following injuries:[4]
- Anterior (and/or posterior) talofibular ligament injury
- Calcaneofibular ligament injury
- Possible peroneal and flexor tendon injuries
- Syndesmotic injury
- On microscopic histopathological analysis, microscopic failure of the collagen fibers characterize ankle sprain when the load and velocity applied to outweigh the mechanical strength of the ligament and speed of a corrective muscle reflex.[5]
Causes
A lateral ankle sprain occurs when the ankle is inverted beyond the elastic limits of its supporting structures causing acute ankle pathology.
- Ankle sprain should be differentiated from (click on the disease name to read more):[6]
- Tendon pathologies: Tendon rupture, ITiFi ligament tear.
- Joint pathologies: Joint effusion, and chronic osteoarthritis.
- Fractures: of the low fibula, Diaphyseal fibula, medial malleolus, postmedial talar process, anterior calcaneal process, os peronei, fifth metatarsal,
- Microfractures: of the cuboid, calcaneum, and tibia.
- Stress fracture
- Subluxation
- Impingement syndrome, sinus tarsi syndrome, tarsal tunnel syndrome, Talar neck avulsion, peroneal groove pathology, peroneal tenosynovitis.
- Muscle pathologies: Split peroneus brevis, peroneus longus, tibialis anterior tear, tibialis posterior dislocation, and flexor digitorum brevis tear.
Epidemiology and Demographics
- The prevalence of ankle sprain is approximately [number or range] per 100,000 individuals worldwide. The most common injuries suffered from during athletic/recreational activities is lateral ankle sprains.[7][8][9]
- The indoor/court sports has a "cumulative incidence rate of 7 per 1,000 exposures or 1.37 per 1,000 athlete exposures and 4.9 per 1,000 h".[10]
Age
- A systematic review and meta-analyses of prospective studies reported that children compared with adolescents and adults are more likely to sustain an ankle sprain.[10]
Gender
- A systematic review and meta-analyses of prospective studies reported that females are more commonly affected with ankle sprain than males.[10]
Race
- There is no racial predilection for ankle sprain.
Risk Factors
- A study describing the common risk factors for development of ankle sprain among recreational basketball players reported having a previous history of ankle injury, wearing shoes with air cells in the heel, and not stretching before the game to be the common risk factors.[11]
Natural History, Complications and Prognosis
- The majority of patients with ankle sprain may remain asymptomatic.
- Early clinical features include tenderness, swelling, and ecchymosis over the anterior talofibuar and calcaneofibular ligaments. Although the patient may be asymptomatic depending upon the extent of injury.
- If left untreated patients with ankle sprain may progress to develop balance problems due to proprioception deficits. [12].
- Common complications of ankle sprain include chronic pain, joint instability, arthritis.[13]
- Prognosis is generally good but acute ankle sprains have been reported to have a high recurrence rate and may also lead to chronic ankle instability.[14]
Diagnosis
Diagnostic Criteria
- The diagnosis of most ankle sprains is made in the light of history of acute ankle trauma and examination findings. Diagnostic imaging is unnecessary although ultrasound may help assess the extent of tendon injury.[15][2]
Symptoms
- Acute injuries may not demonstrate any signs and symptoms. Ask the patient to describe injury mechanism. Most sprains involve ankle inversion with some plantar flexion and suggest lateral ligament injury. Another mechanism, such as dorsiflexion, eversion suggest some other ligament involvement.[1]
Physical Examination
- Patients with ankle sprain usually appear fine. But, the patient may be in distress depending upon the intensity of pain.
- Physical examination of a typical lateral ankle sprain may be remarkable for:
- Tenderness, swelling, and ecchymosis over anterior talofibuar and calcaneofibular ligaments. Swelling and bruising of the whole foot and toe may be demonstrated if no proper treatment has been applied and the patient has been ambulating.[1]
- The patient should be assessed for the degree of instability, site, pain intensity, and an evaluation of neurovascular status.[16]
Laboratory Findings
- There are no specific laboratory findings associated with ankle sprain.
Electrocardiogram
- There are no ECG findings associated with ankle sprain.
X-ray
- An x-ray may be helpful in the diagnosis of ankle sprain. The Ottawa criteria (100% sensitivity) helps indicate of the radiography is indicated. According to the criteria, in case of pain in the malleolar or midfoot region, or tenderness of the bone over the potential fracture region, or weight bearing inability for four steps right after the injury warrants radiography.[17][18]
- Lateral, anteroposterior, and mortise views of the ankle help visualize the lesion.
Ultrasound
- Ultrasound findings include thickening and hypoechogenicity of the affected ligament demonstrate a sprain.[4]
CT scan
- CT scan may be helpful in the diagnosis of ankle sprain. Findings on CT scan suggestive of sprain include thickening, thinning, irregularity, discontinuity, or an absent ligament. Sometimes bony avulsions can be visible.[4]
MRI
- An ankle MRI may be helpful for ankle injuries involving crepitus or locking, as these symptoms may indicate a displaced osteochondral fragment.[19]
- An MRI may help identify syndesmosis sprains and peroneal tendon involvement.[20]
Treatment
- Although treatment decisions must be made on an individual basis, functional support for most ankle sprains is the first step.[21] Brace, tape, elastic bandage, or soft cast are preferred over immobilization.[22] It gives the leg an exercise and yet keeps the damaged part from moving. Crutches and air-braces while conventionally used, are currently out of vogue.
- Immediately following the injury it is important the follow the PRICE protocol – Protection, Rest, Ice, Compression, and Elevation (also known as RICE: Rest, Ice, Compress, and Elevate).[23]
- Cold therapy for 12 to 20 minutes together with compression until the swelling settles or 48 hours, is found to be helpful.[24][25][23]
- Severe ankle sprains should be assessed by an orthopedic specialist, although physical therapy is extremely effective for most sprained ankles.
- The evidence of use of ultrasound, LASER, and manual therapy (such as anteroposterior glide of the talus, Mulligan’s mobilization with movement, chiropractic mortise adjustment technique) for reducing swelling and pain is at various levels.[26][27][28][21]
Medical Therapy
Surgery
- Surgical repair can be performed for patients with ruptured ankle ligaments. Operative treatment has been shown to have a better long-term outcome for residual pain, recurrent sprains and stability in a randomised clinical trial.[31]
Prevention
- Effective measures for the primary prevention of the ankle sprain include warming up before the sports.
Related Chapters
References
- ↑ 1.0 1.1 1.2 Tiemstra JD (June 2012). "Update on acute ankle sprains". Am Fam Physician. 85 (12): 1170–6. PMID 22962897.
- ↑ 2.0 2.1 McGovern RP, Martin RL (2016). "Managing ankle ligament sprains and tears: current opinion". Open Access J Sports Med. 7: 33–42. doi:10.2147/OAJSM.S72334. PMC 4780668. PMID 27042147.
- ↑ Hur ES, Bohl DD, Lee S (August 2020). "Lateral Ligament Instability: Review of Pathology and Diagnosis". Curr Rev Musculoskelet Med. 13 (4): 494–500. doi:10.1007/s12178-020-09641-z. PMC 7340720 Check
|pmc=value (help). PMID 32495041 Check|pmid=value (help). - ↑ 4.0 4.1 4.2 "Lateral ankle sprain | Radiology Reference Article | Radiopaedia.org".
- ↑ Dubin JC, Comeau D, McClelland RI, Dubin RA, Ferrel E (September 2011). "Lateral and syndesmotic ankle sprain injuries: a narrative literature review". J Chiropr Med. 10 (3): 204–19. doi:10.1016/j.jcm.2011.02.001. PMC 3259913. PMID 22014912.
- ↑ Meyr, Andrew (2008). Pain management. Philadelphia, Pa: Elsevier Saunders. ISBN 1416063412.
- ↑ Fernandez WG, Yard EE, Comstock RD (July 2007). "Epidemiology of lower extremity injuries among U.S. high school athletes". Acad Emerg Med. 14 (7): 641–5. doi:10.1197/j.aem.2007.03.1354. PMID 17513688.
- ↑ Hootman JM, Dick R, Agel J (2007). "Epidemiology of collegiate injuries for 15 sports: summary and recommendations for injury prevention initiatives". J Athl Train. 42 (2): 311–9. PMC 1941297. PMID 17710181.
- ↑ Hubbard TJ, Wikstrom EA (July 2010). "Ankle sprain: pathophysiology, predisposing factors, and management strategies". Open Access J Sports Med. 1: 115–22. doi:10.2147/oajsm.s9060. PMC 3781861. PMID 24198549.
- ↑ 10.0 10.1 10.2 Doherty C, Delahunt E, Caulfield B, Hertel J, Ryan J, Bleakley C (January 2014). "The incidence and prevalence of ankle sprain injury: a systematic review and meta-analysis of prospective epidemiological studies". Sports Med. 44 (1): 123–40. doi:10.1007/s40279-013-0102-5. PMID 24105612.
- ↑ McKay GD, Goldie PA, Payne WR, Oakes BW (April 2001). "Ankle injuries in basketball: injury rate and risk factors". Br J Sports Med. 35 (2): 103–8. doi:10.1136/bjsm.35.2.103. PMC 1724316. PMID 11273971.
- ↑ Akbari M, Karimi H, Farahini H, Faghihzadeh S (2006). "Balance problems after unilateral lateral ankle sprains". J Rehabil Res Dev. 43 (7): 819–24. doi:10.1682/jrrd.2006.01.0001. PMID 17436168.
- ↑ Martin B (April 2008). "Ankle sprain complications: MRI evaluation". Clin Podiatr Med Surg. 25 (2): 203–47, vi. doi:10.1016/j.cpm.2007.12.004. PMID 18346591.
- ↑ Herzog MM, Kerr ZY, Marshall SW, Wikstrom EA (June 2019). "Epidemiology of Ankle Sprains and Chronic Ankle Instability". J Athl Train. 54 (6): 603–610. doi:10.4085/1062-6050-447-17. PMC 6602402 Check
|pmc=value (help). PMID 31135209. - ↑ 15.0 15.1 Vuurberg G, Hoorntje A, Wink LM, van der Doelen B, van den Bekerom MP, Dekker R, van Dijk CN, Krips R, Loogman M, Ridderikhof ML, Smithuis FF, Stufkens S, Verhagen E, de Bie RA, Kerkhoffs G (August 2018). "Diagnosis, treatment and prevention of ankle sprains: update of an evidence-based clinical guideline". Br J Sports Med. 52 (15): 956. doi:10.1136/bjsports-2017-098106. PMID 29514819. Vancouver style error: initials (help)
- ↑ Meyr, Andrew (2008). Pain management. Philadelphia, Pa: Elsevier Saunders. ISBN 1416063412.
- ↑ Bachmann LM, Kolb E, Koller MT, Steurer J, ter Riet G (February 2003). "Accuracy of Ottawa ankle rules to exclude fractures of the ankle and mid-foot: systematic review". BMJ. 326 (7386): 417. doi:10.1136/bmj.326.7386.417. PMC 149439. PMID 12595378.
- ↑ Dowling S, Spooner CH, Liang Y, Dryden DM, Friesen C, Klassen TP, Wright RB (April 2009). "Accuracy of Ottawa Ankle Rules to exclude fractures of the ankle and midfoot in children: a meta-analysis". Acad Emerg Med. 16 (4): 277–87. doi:10.1111/j.1553-2712.2008.00333.x. PMID 19187397.
- ↑ Wolfe MW, Uhl TL, Mattacola CG, McCluskey LC (January 2001). "Management of ankle sprains". Am Fam Physician. 63 (1): 93–104. PMID 11195774.
- ↑ Lazarus ML (July 1999). "Imaging of the foot and ankle in the injured athlete". Med Sci Sports Exerc. 31 (7 Suppl): S412–20. doi:10.1097/00005768-199907001-00002. PMID 10416542.
- ↑ 21.0 21.1 Lin CW, Hiller CE, de Bie RA (March 2010). "Evidence-based treatment for ankle injuries: a clinical perspective". J Man Manip Ther. 18 (1): 22–8. doi:10.1179/106698110X12595770849524. PMC 3103112. PMID 21655420.
- ↑ Kerkhoffs GM, Rowe BH, Assendelft WJ, Kelly K, Struijs PA, van Dijk CN (2002). "Immobilisation and functional treatment for acute lateral ankle ligament injuries in adults". Cochrane Database Syst Rev (3): CD003762. doi:10.1002/14651858.CD003762. PMID 12137710.
- ↑ 23.0 23.1 van den Bekerom MP, Struijs PA, Blankevoort L, Welling L, van Dijk CN, Kerkhoffs GM (2012). "What is the evidence for rest, ice, compression, and elevation therapy in the treatment of ankle sprains in adults?". J Athl Train. 47 (4): 435–43. doi:10.4085/1062-6050-47.4.14. PMC 3396304. PMID 22889660.
- ↑ Sloan JP, Hain R, Pownall R (March 1989). "Clinical benefits of early cold therapy in accident and emergency following ankle sprain". Arch Emerg Med. 6 (1): 1–6. doi:10.1136/emj.6.1.1. PMC 1285549. PMID 2712981.
- ↑ Airaksinen O, Kolari PJ, Miettinen H (May 1990). "Elastic bandages and intermittent pneumatic compression for treatment of acute ankle sprains". Arch Phys Med Rehabil. 71 (6): 380–3. PMID 2334279.
- ↑ Eisenhart AW, Gaeta TJ, Yens DP (September 2003). "Osteopathic manipulative treatment in the emergency department for patients with acute ankle injuries". J Am Osteopath Assoc. 103 (9): 417–21. PMID 14527076.
- ↑ Green T, Refshauge K, Crosbie J, Adams R (April 2001). "A randomized controlled trial of a passive accessory joint mobilization on acute ankle inversion sprains". Phys Ther. 81 (4): 984–94. PMID 11276181.
- ↑ Collins N, Teys P, Vicenzino B (May 2004). "The initial effects of a Mulligan's mobilization with movement technique on dorsiflexion and pain in subacute ankle sprains". Man Ther. 9 (2): 77–82. doi:10.1016/S1356-689X(03)00101-2. PMID 15040966.
- ↑ Massey T, Derry S, Moore RA, McQuay HJ (June 2010). "Topical NSAIDs for acute pain in adults". Cochrane Database Syst Rev (6): CD007402. doi:10.1002/14651858.CD007402.pub2. PMC 4163964. PMID 20556778.
- ↑ Morán M (1991). "Double-blind comparison of diclofenac potassium, ibuprofen and placebo in the treatment of ankle sprains". J Int Med Res. 19 (2): 121–30. doi:10.1177/030006059101900205. PMID 1864448.
- ↑ Pijnenburg AC, Bogaard K, Krips R, Marti RK, Bossuyt PM, van Dijk CN (May 2003). "Operative and functional treatment of rupture of the lateral ligament of the ankle. A randomised, prospective trial". J Bone Joint Surg Br. 85 (4): 525–30. doi:10.1302/0301-620x.85b4.13928. PMID 12793557.
Template:Dislocations, sprains and strains Template:WH Template:WS