Thalassemia laboratory findings
|
Thalassemia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Thalassemia laboratory findings On the Web |
|
American Roentgen Ray Society Images of Thalassemia laboratory findings |
|
Risk calculators and risk factors for Thalassemia laboratory findings |
Please help WikiDoc by adding more content here. It's easy! Click here to learn about editing.
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Shyam Patel [2]
Overview
Laboratory findings in patients with thalassemia include anemia with microcytosis, abnormal bands on hemoglobin electrophoresis, and abnormal peripheral blood smear findings. Sequencing of the globin genes will reveal mutations that lead to defective globin production. In the case of hemolysis from thalassemia, laboratory findings include elevated LDH, elevated total bilirubin, elevated indirect bilirubin, high reticulocyte count, and low haptoglobin. Importantly, the range of laboratory findings is quite diverse depending on the severity of the disease.
Laboratory Findings
- Low hemoglobin: Low hemoglobin, or anemia, is always found in patients with thalassemia. This is a defining and required laboratory feature of all thalassmias.
- Elevated red blood cell mass: This is a somewhat unique feature of thalassemia. A low hemoglobin plus elevated red blood cell mass should prompt a clinician to consider thalassemia as the cause of anemia. In contrast, patients with iron-deficiency anemia have low hemoglobin but do not have elevated red blood cell mass.
- Microcytosis: Red blood cells in thalassemia have low mean corpuscular volume (MCV), typically less than 80 femtoliters. This is similar to the MCV in iron-deficiency anemia.[1]
- Hypochromasia: Red blood cells in thalassemia have central pallor, similar to red blood cells in iron-deficiency anemia.[1]
- Elevated lactate dehydrogenase (LDH): This is due to hemolysis, in which intracellular contents (such as LDH) are released into the circulation.
- Indirect, or unconjugated, hyperbilirubinemia: This is due to hemolysis, in which breaskdown products of heme are released into the bloodstream.
- Low haptoglobin: This is due to hemolysis, in which free hemoglobin in the circulation binds to and reduces the level of haptoglobin.
- Elevated reticulocyte count: This is due to a bone marrow compensatory response to low hemoglobin levels from thalassemia. Reticulocytes are precursors of red blood cells and thus an elevated reticulocyte count signifies an adequate compensatory attempt to produce more red blood cells.
- Abnormal bands on hemoglobin electrophoresis: Hemoglobin electrophoresis is the gold standard diagnostic test for thalassemia. In normal persons, a hemoglobin electrophoresis will show a strong band corresponding to hemoglobin A (tetramer of 2 alpha-globin chains and 2 beta-globin chains) and a weak band corresponding to hemoglobin A2 (tetramer of 2 alpha-globin chains and 2 delta-globin chains). In thalassemia, various other bands can be present on electrophoresis. These include tetramers of gamma-globin chains (such as in Hb Barts) or tetramers of beta-globin chains (such as in HbH disease).
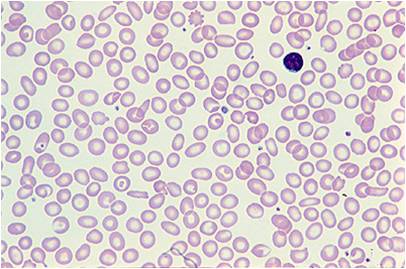
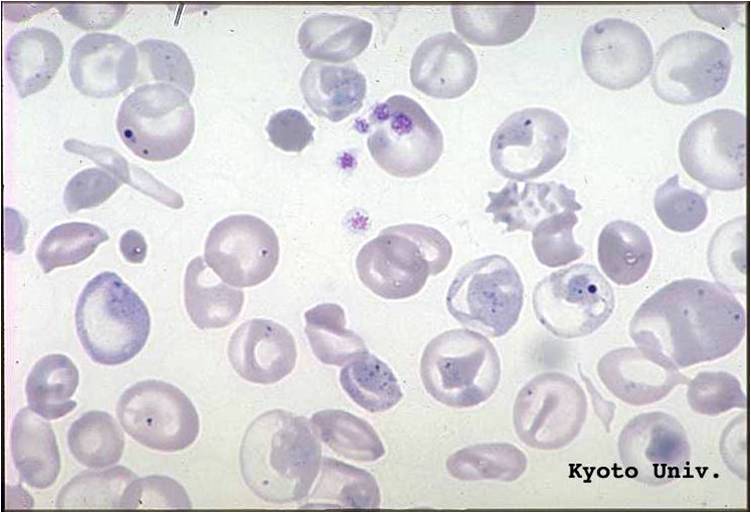
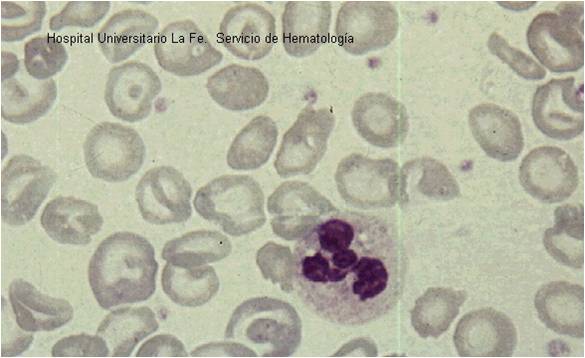
- Abnormal cells on peripheral blood smear: The peripheral blood smear is perhaps the most inexpensive laboratory test that can accurately lead to a diagnosis of thalassemia. Patients with thalassemia have target cells and hypochromic (low color) and microcytic (small-sized) red blood cells.
- Mutations in alpha-globin on DNA sequencing: This is a specialized test that can definitively determine the presence of alpha-thalassemia. Sequencing of the alpha-globin chain from peripheral blood cells can help diagnose alpha-thalassemia. This laboratory test is more expensive that the other tests. This laboratory findings is pathognomonic for alpha-thalassemia. Deletions or insertions are more common in the alpha-globin gene compared to the beta-globin gene.
- Mutations in beta-globin on DNA sequencing: This is a specialized test that can definitively determine the presence of beta-thalassemia. Sequencing of the beta-globin chain from peripheral blood cells can help diagnose beta-thalassemia. This laboratory test is more expensive that the other tests. This laboratory findings is pathognomonic for beta-thalassemia. Point mutations (substitutions) are more common in the beta-globin gene compared to the alpha-globin gene.
Peripheral Smear
(Images shown below are courtesy of Melih Aktan MD, Istanbul Medical Faculty - Turkey, and Kyoto University - Japan, and Hospital Universitario La Fe Servicio Hematologia)
References
- ↑ 1.0 1.1 Chui DH, Cunningham MJ, Luo HY, Wolfe LC, Neufeld EJ, Steinberg MH (2006). "Screening and counseling for thalassemia". Blood. 107 (4): 1735–7. doi:10.1182/blood-2005-09-3557. PMC 1895412. PMID 16461765.