Selegiline (transdermal)
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Turky Alkathery, M.D. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
SUICIDAL THOUGHTS AND BEHAVIORS
See full prescribing information for complete Boxed Warning.
Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a trend toward reduced risk with antidepressant use in patients aged 65 and older [see WARNINGS AND PRECAUTIONS (5.1)].
|
Overview
Selegiline (transdermal) is a monoamine oxidase inhibitor (MAOI) that is FDA approved for the treatment of major depressive disorder (MDD). There is a Black Box Warning for this drug as shown here. Common adverse reactions include application site reaction, headache, insomnia, diarrhea, dry mouth, dyspepsia, rash, pharyngitis and sinusitis.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indications
EMSAM (selegiline transdermal system) is a monoamine oxidase inhibitor (MAOI) indicated for the treatment of major depressive disorder (MDD). The efficacy of EMSAM in the treatment of major depressive disorder was established in two short term (6-week and 8-week) trials of outpatients with major depressive disorder. Efficacy was studied in two short term studies and one maintenance study
Dosage
2.1 Initial Treatment EMSAM should be applied to dry, intact skin on the upper torso (below the neck and above the waist), upper thigh or the outer surface of the upper arm once every 24 hours. The recommended starting dose and target dose for EMSAM is 6 mg per 24 hours. EMSAM has been systematically evaluated and shown to be effective in a dose range of 6 mg per 24 hours to 12 mg per 24 hours. However, the trials were not designed to assess if higher doses are more effective than the lowest effective dose of 6 mg per 24 hours. Based on clinical judgment, if dose increases are indicated for individual patients, they should occur in dose increments of 3 mg per 24 hours (up to a maximum dose of 12 mg per 24 hours) at intervals of no less than 2 weeks. Full antidepressant effect may be delayed.
Patients should be informed that tyramine-rich foods and beverages should be avoided beginning on the first day of EMSAM 9 mg per 24 hours or 12 mg per 24 hours treatment and should continue to be avoided for 2 weeks after a dose reduction to EMSAM 6 mg per 24 hours or following the discontinuation of EMSAM 9 mg per 24 hours or 12 mg per 24 hours [see WARNINGS AND PRECAUTIONS (5.3)].
2.2 Maintenance Treatment It is generally agreed that episodes of depression require several months or longer of sustained pharmacologic therapy. Maintenance of efficacy in depressed patients on therapy with EMSAM at a dose of 6 mg per 24 hours after achieving a responder status for an average duration of about 25 days was demonstrated in a controlled trial [see INDICATIONS AND USAGE (1) and CLINICAL STUDIES (14.1)].
The physician who elects to use EMSAM for extended periods should periodically re-evaluate the long-term usefulness of the drug for the individual patient.
2.3 Dietary Modifications Required for Patients Taking EMSAM 9 mg per 24 hours and 12 mg per 24 hours EMSAM (selegiline transdermal system) contains a monoamine oxidase inhibitor (MAOI). MAOIs including EMSAM combined with a high tyramine diet may cause a hypertensive crisis. A hypertensive crisis can be a life-threatening condition [see WARNINGS AND PRECAUTIONS (5.3)].
The foods and beverages listed in Table 5 should be avoided beginning on the first day of EMSAM 9 mg per 24 hours or 12 mg per 24 hours treatment, and should continue to be avoided for 2 weeks after a dose reduction to EMSAM 6 mg per 24 hours or following the discontinuation of EMSAM 9 mg per 24 hours or 12 mg per 24 hours.
DOSAGE FORMS AND STRENGTHS
EMSAM (selegiline transdermal system) is supplied as 6 mg per 24 hours (20 mg per 20 cm2), 9 mg per 24 hours (30 mg per 30 cm2) and 12 mg per 24 hours (40 mg per 40 cm2) transdermal systems (TDS).
EMSAM 6 mg per 24 hours is a translucent TDS printed with ‘EMSAM® 6mg/24h’. EMSAM 9 mg per 24 hours is a translucent TDS printed with ‘EMSAM® 9mg/24h’. EMSAM 12 mg per 24 hours is a translucent TDS printed with ‘EMSAM® 12mg/24h’.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Selegiline (transdermal) in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Selegiline (transdermal) in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Selegiline (transdermal) FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Selegiline (transdermal) in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Selegiline (transdermal) in pediatric patients.
Contraindications
EMSAM (selegiline transdermal system) is contraindicated with selective serotonin reuptake inhibitors (SSRIs, e.g., fluoxetine, sertraline, and paroxetine); serotonin and norepinephrine reuptake inhibitors (SNRIs, e.g., venlafaxine and duloxetine); the tricyclic antidepressants clomipramine and imipramine, the opiate analgesics meperidine, tramadol, methadone, pentazocine, and propoxyphene; and the antitussive agent dextromethorphan because of a risk of serotonin syndrome when EMSAM is used with these agents [see WARNINGS AND PRECAUTIONS (5.2) and DRUG INTERACTIONS (7.1)]. Carbamazepine is contraindicated with EMSAM because of a possible increased risk of hypertensive crisis [see WARNINGS AND PRECAUTIONS (5.3) and CLINICAL PHARMACOLOGY (12.3)]. After stopping treatment with drugs contraindicated with EMSAM, a time period equal to 4 to 5 half-lives (approximately one week) of the drug or any active metabolite should elapse before starting therapy with EMSAM. Because of the long half-life of fluoxetine and its active metabolite, at least 5 weeks should elapse between discontinuation of fluoxetine and initiation of treatment with EMSAM. At least 2 weeks should elapse after stopping EMSAM before starting therapy with any drug that is contraindicated with EMSAM. EMSAM is contraindicated in patients less than 12 years of age because of the potential for a hypertensive crisis [see USE IN SPECIFIC POPULATIONS (8.4) and CLINICAL PHARMACOLOGY (12.3)]. EMSAM is contraindicated in patients with pheochromocytoma because MAOIs may precipitate a hypertensive crisis in such patients.
Warnings
|
SUICIDAL THOUGHTS AND BEHAVIORS
See full prescribing information for complete Boxed Warning.
Antidepressants increased the risk of suicidal thoughts and behavior in children, adolescents, and young adults in short-term studies. These studies did not show an increase in the risk of suicidal thoughts and behavior with antidepressant use in patients over age 24; there was a trend toward reduced risk with antidepressant use in patients aged 65 and older [see WARNINGS AND PRECAUTIONS (5.1)].
|
5.1 Clinical Worsening and Suicide Risk Patients with major depressive disorder (MDD), both adult and pediatric, may experience worsening of their depression and/or the emergence of suicidal ideation and behavior (suicidality) or unusual changes in behavior, whether or not they are taking antidepressant medications, and this risk may persist until significant remission occurs. Suicide is a known risk of depression and certain other psychiatric disorders, and these disorders themselves are the strongest predictors of suicide. There has been a long-standing concern, however, that antidepressants may have a role in inducing worsening of depression and the emergence of suicidality in certain patients during the early phases of treatment. Pooled analyses of short-term placebo-controlled trials of antidepressant drugs (selective serotonin reuptake inhibitors [SSRIs] and others) showed that these drugs increase the risk of suicidal thinking and behavior (suicidality) in children, adolescents, and young adults (ages 18 to 24) with major depressive disorder (MDD) and other psychiatric disorders. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a trend toward risk reduction with antidepressants compared to placebo in adults aged 65 and older.
The pooled analyses of placebo-controlled trials in children and adolescents with MDD, obsessive compulsive disorders (OCD), or other psychiatric disorders included a total of 24 short-term trials of nine antidepressant drugs in over 4,400 patients. The pooled analyses of placebo-controlled trials in adults with MDD or other psychiatric disorders included a total of 295 short-term trials (median duration of two months) of 11 antidepressant drugs in over 77,000 patients. There was considerable variation in risk of suicidality among drugs, but a tendency toward an increase in the younger patients for almost all drugs studied. There were differences in absolute risk of suicidality across the different indications, with the highest incidence in MDD. The risk differences (drug vs. placebo), however, were relatively stable within age strata and across indications. These risk differences (drug-placebo difference in the number of cases of suicidality per 1,000 patients treated) are provided in Table 1.\
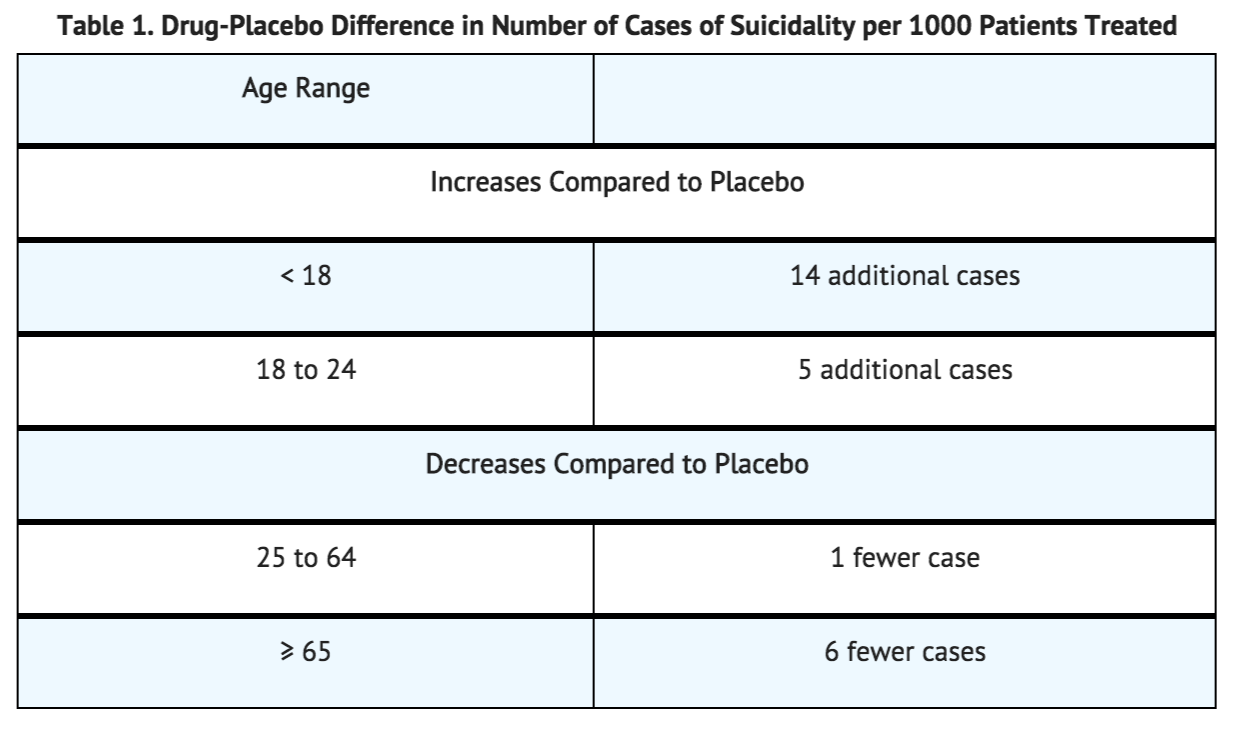
No suicides occurred in any of the pediatric trials. There were suicides in the adult trials, but the number was not sufficient to reach any conclusion about drug effect on suicide.
It is unknown whether the suicidality risk extends to longer term use, i.e., beyond several months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with depression that the use of antidepressants can delay the recurrence of depression.
All patients being treated with antidepressants for any indication should be monitored appropriately and observed closely for clinical worsening, suicidality, and unusual changes in behavior, especially during the initial few months of a course of drug therapy, or at times of dose changes, either increases or decreases.
The following symptoms anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, and mania have been reported in adult and pediatric patients being treated with antidepressants for MDD as well as for other indications, both psychiatric and nonpsychiatric. Although a causal link between the emergence of such symptoms and either the worsening of depression and/or the emergence of suicidal impulses has not been established, there is concern that such symptoms may represent precursors to emerging suicidality.
Consideration should be given to changing the therapeutic regimen, including possibly discontinuing the medication, in patients whose depression is persistently worse, or who are experiencing emergent suicidality or symptoms that might be precursors to worsening depression or suicidality, especially if these symptoms are severe, abrupt in onset, or were not part of the patient’s presenting symptoms.
Families and caregivers of patients being treated with antidepressants for MDD or other indications, both psychiatric and nonpsychiatric, should be alerted about the need to monitor patients for the emergence of agitation, irritability, unusual changes in behavior, and the other symptoms described above, as well as the emergence of suicidality, and to report such symptoms immediately to healthcare providers. Such monitoring should include daily observation by families and caregivers.
Screening Patients for Bipolar Disorder
A major depressive episode may be the initial presentation of bipolar disorder. It is generally believed (though not established in controlled trials) that treating such an episode with an antidepressant alone may increase the likelihood of precipitation of a mixed/manic episode in patients at risk for bipolar disorder. Whether any of the symptoms described above represent such a conversion is unknown. However, prior to initiating treatment with an antidepressant, patients with depressive symptoms should be adequately screened to determine if they are at risk for bipolar disorder; such screening should include a detailed psychiatric history, including a family history of suicide, bipolar disorder, and depression. It should be noted that EMSAM is not approved for use in treating bipolar depression.
5.2 Serotonin Syndrome The development of a potentially life-threatening serotonin syndrome has been reported with concomitant use of MAOIs, such as EMSAM, with serotonergic drugs. These reactions have also been reported in patients who have discontinued serotonergic drugs and then subsequently started an MAOI [see CONTRAINDICATIONS (4)].
Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular changes (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
Patients should be monitored for the emergence of serotonin syndrome. Treatment with EMSAM and any concomitant serotonergic agents should be discontinued immediately if the above events occur and supportive treatment should be initiated.
5.3 Blood Pressure Elevation Tyramine-Induced Hypertensive Crisis
EMSAM inhibits the catabolism of dietary amines, such as tyramine, and has the potential to produce a hypertensive crisis following the ingestion of tyramine-rich foods or beverages [see DRUG INTERACTIONS (7.2) and CLINICAL PHARMACOLOGY (12.2)].
Hypertensive crises, which in some cases may be fatal, are characterized by some or all of the following symptoms: occipital headache which may radiate frontally, palpitation, neck stiffness or soreness, nausea, vomiting, sweating (sometimes with fever and sometimes with cold, clammy skin), dilated pupils, and photophobia. Either tachycardia or bradycardia may be present and can be associated with constricting chest pain. Intracranial bleeding has been reported in association with the increase in blood pressure. Patients should be instructed as to the signs and symptoms of severe hypertension and advised to seek immediate medical attention if these signs or symptoms are present.
If a hypertensive crisis occurs, EMSAM should be discontinued immediately and therapy to lower blood pressure should be instituted immediately. Fever should be managed by means of external cooling. Patients must be closely monitored until symptoms have stabilized.
To prevent a hypertensive crisis, patients receiving treatment with EMSAM 9 mg per 24 hours or EMSAM 12 mg per 24 hours should follow the advice regarding a low tyramine diet described in Table 5 under Dietary Modifications Required for Patients Taking EMSAM 9 mg per 24 hours and 12 mg per 24 hours [see DRUG INTERACTIONS (7.2)].
Blood Pressure Elevation Related to Concomitant Medication
Carbamazepine is contraindicated with EMSAM because carbamazepine has been shown to significantly elevate selegiline levels, which may increase the risk of a hypertensive crisis [see CONTRAINDICATIONS (4) and DRUG INTERACTIONS (7.4)].
The use of EMSAM with adrenergic drugs or buspirone may produce substantial increases in blood pressure. Therefore, monitor blood pressure if EMSAM is used with any of the following drugs: buspirone, amphetamines, or cold products or weight-reducing preparations that contain sympathomimetic amines (e.g., pseudoephedrine, phenylephrine, phenylpropanolamine, and ephedrine).
5.4 Activation of Mania/Hypomania During Phase III trials, a manic reaction occurred in 8 out of 2,036 (0.4%) patients treated with EMSAM. Activation of mania/hypomania can occur in a small proportion of patients with major depressive disorder treated with antidepressants. EMSAM should be used cautiously in patients with a history of mania.
5.5 External Heat The effect of direct heat applied to the EMSAM patch on the bioavailability of selegiline has not been studied. However, in theory, heat may result in an increase in the amount of selegiline absorbed from the EMSAM patch and produce elevated serum levels of selegiline. Patients should be advised to avoid exposing the EMSAM application site to external sources of direct heat, such as heating pads or electric blankets, heat lamps, saunas, hot tubs, heated water beds, and prolonged direct sunlight.
Adverse Reactions
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
Patient Exposure
The premarketing development program for EMSAM included selegiline exposures in patients and/or normal subjects from two different groups of studies: 702 healthy subjects in clinical pharmacology/pharmacokinetics studies and 2,036 exposures from patients in controlled and uncontrolled major depressive disorder clinical trials. The conditions and duration of treatment with EMSAM varied and included double-blind, open-label, fixed-dose, and dose titration studies of short-term and longer-term exposures. Safety was assessed by monitoring adverse reactions, physical examinations, vital signs, body weights, laboratory analyses, and ECGs.
Adverse reactions during exposure were obtained primarily by general inquiry and recorded by clinical investigators. In the tables and tabulations that follow, standard COSTART terminology has been used to classify reported adverse reactions. The stated frequencies of adverse reactions represent the proportion of individuals who experienced, at least once, a treatment-emergent adverse reaction of the type listed. A reaction was considered treatment-emergent if it occurred for the first time or worsened while receiving therapy following baseline evaluation.
Adverse Reactions Leading To Discontinuation of Treatment
Among 817 MDD patients treated with EMSAM at doses of either 3 mg per 24 hours (151 patients), 6 mg per 24 hours (550 patients) or 6 mg per 24 hours, 9 mg per 24 hours, and 12 mg per 24 hours (116 patients) in placebo-controlled trials of up to 8 weeks in duration, 7.1% discontinued treatment due to an adverse reaction as compared with 3.6% of 668 patients receiving placebo. The only adverse reaction associated with discontinuation, in at least 1% of EMSAM-treated patients at a rate at least twice that of placebo, was application site reaction (2% EMSAM vs. 0% placebo).
Adverse Reactions Occurring at an Incidence of 2% or More Among EMSAM-Treated Patients
Table 2 enumerates adverse reactions that occurred at an incidence of 2% or more (rounded to the nearest percent) among 817 MDD patients treated with EMSAM in doses ranging from 3 to 12 mg per 24 hours in placebo-controlled trials of up to 8 weeks in duration. Reactions included are those occurring in 2% or more of patients treated with EMSAM and for which the incidence in patients treated with EMSAM was greater than the incidence in placebo-treated patients.
One adverse reaction was associated with a reporting of at least 5% in the EMSAM group, and a rate at least twice that in the placebo group, in the pool of short-term, placebo-controlled studies: application site reactions (see APPLICATION SITE REACTIONS, below). In one such study which utilized higher mean doses of EMSAM than that in the entire study pool, the following reactions met these criteria: application site reactions, insomnia, diarrhea, and pharyngitis.
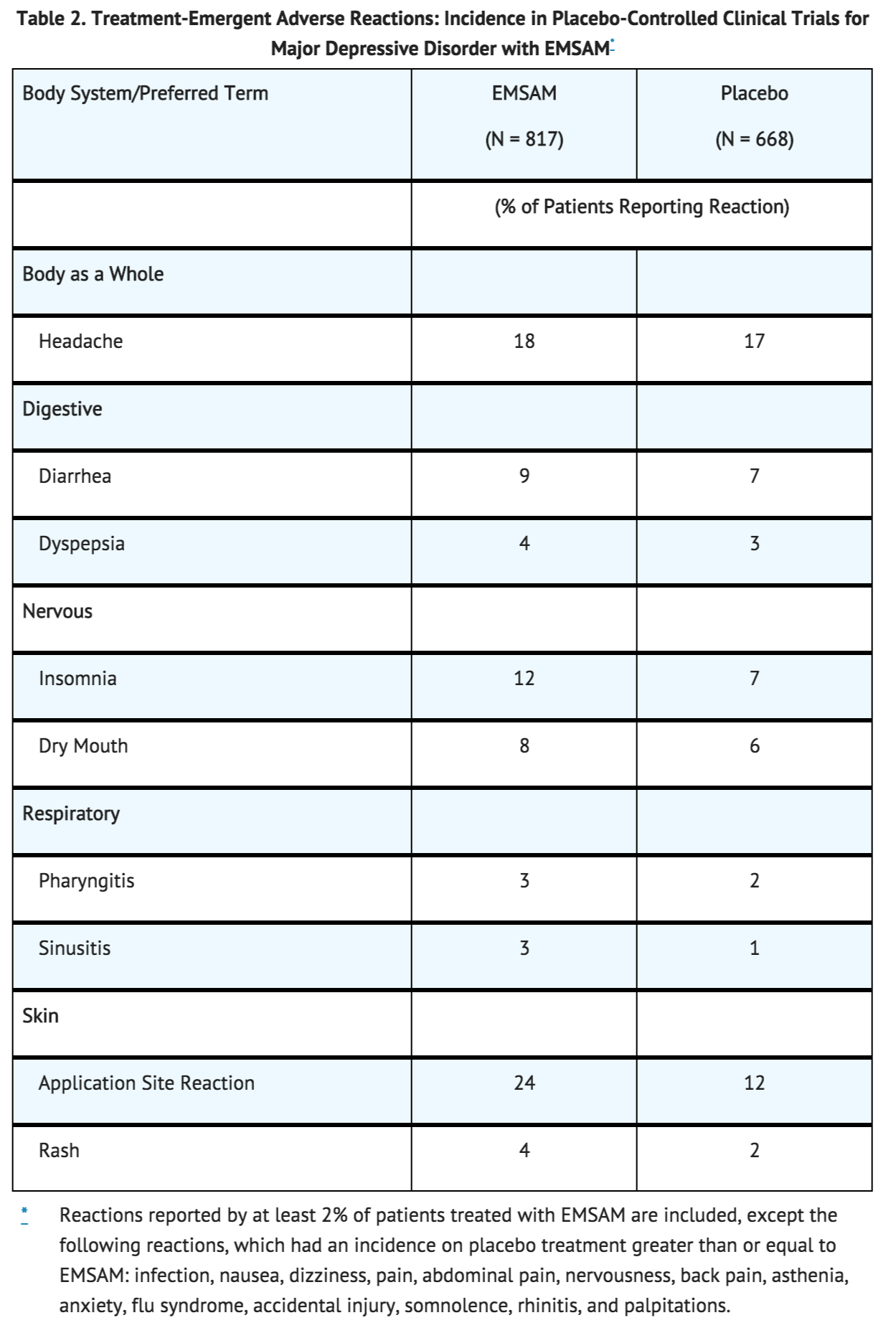
Application Site Reactions
In the pool of short-term, placebo-controlled major depressive disorder studies, application site reactions (ASRs) were reported in 24% of EMSAM-treated patients and 12% of placebo-treated patients. Most ASRs were mild or moderate in severity. ASRs led to dropout in 2% of EMSAM-treated patients and no placebo-treated patients.
In one such study which utilized higher mean doses of EMSAM, ASRs were reported in 40% of EMSAM-treated patients and 20% of placebo-treated patients. Most of the ASRs in this study were described as erythema and most resolved spontaneously, requiring no treatment. When treatment was administered, it most commonly consisted of dermatological preparations of corticosteroids.
Sexual Dysfunction
Although changes in sexual desire, sexual performance, and sexual satisfaction often occur as manifestations of a psychiatric disorder, they may also be a consequence of pharmacologic treatment.
Reliable estimates of the incidence and severity of untoward experiences involving sexual desire, performance, and satisfaction are difficult to obtain, in part because patients and physicians may be reluctant to discuss them. Accordingly, estimates of the incidence of untoward sexual experience and performance cited in product labeling are likely to underestimate their actual incidence. Table 3 shows that the incidence rates of sexual side effects in patients with major depressive disorder are comparable to the placebo rates in placebo-controlled trials.
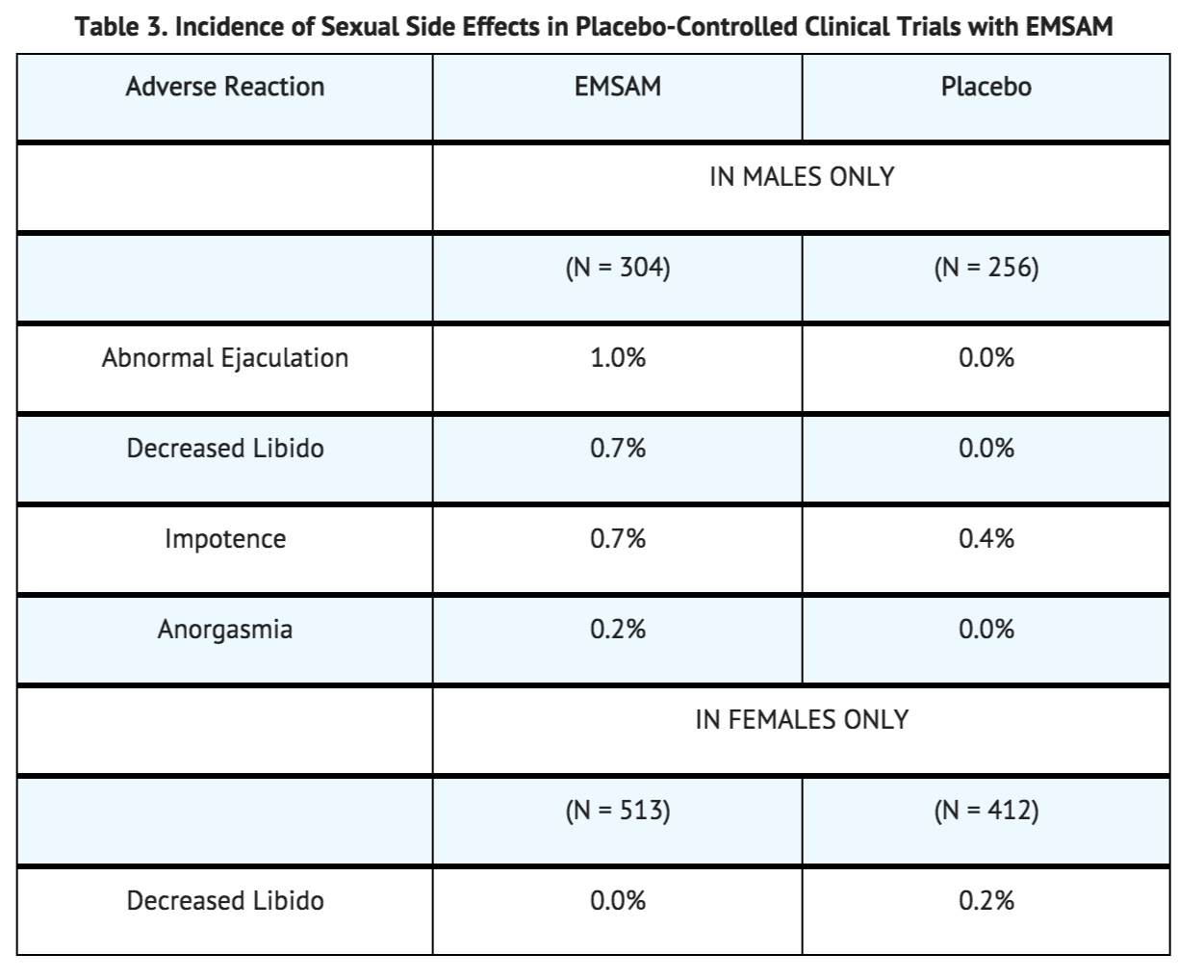
There are no adequately designed studies examining sexual dysfunction with EMSAM treatment.
Vital Sign Changes
EMSAM and placebo groups were compared with respect to (1) mean change from baseline in vital signs (pulse, systolic blood pressure, and diastolic blood pressure), and (2) the incidence of patients meeting criteria for potentially clinically significant changes from baseline in these variables. In the pool of short-term, placebo-controlled major depressive disorder studies, 3.0% of EMSAM-treated patients and 1.5% of placebo-treated patients experienced a low systolic blood pressure, defined as a reading less than or equal to 90 mmHg with a change from baseline of at least 20 mmHg. In one study which utilized higher mean doses of EMSAM, 6.2% of EMSAM-treated patients and no placebo-treated patients experienced a low standing systolic blood pressure by these criteria.
In the pool of short-term major depressive disorder trials, 9.8% of EMSAM-treated patients and 6.7% of placebo-treated patients experienced a notable orthostatic change in blood pressure, defined as a decrease of at least 10 mmHg in mean blood pressure with postural change.
Weight Changes
In placebo-controlled studies (6 to 8 weeks), the incidence of patients who experienced at least 5% weight gain or weight loss is shown in Table 4.
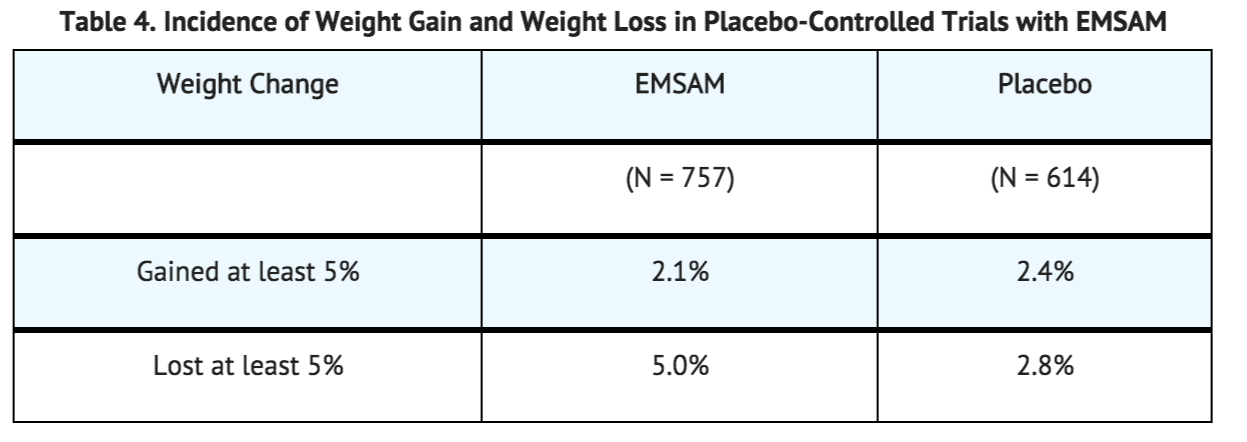
In these trials, the mean change in body weight among EMSAM-treated patients was a 1.2 lbs loss compared to 0.3 lbs gain in placebo-treated patients.
Laboratory Changes
EMSAM and placebo groups were compared with respect to (1) mean change from baseline in various serum chemistry, hematology, and urinalysis variables, and (2) the incidence of patients meeting criteria for potentially clinically significant changes from baseline in these variables. These analyses revealed no clinically important changes in laboratory test parameters associated with EMSAM.
Electrocardiogram Changes
Electrocardiograms (ECGs) from EMSAM (N = 817) and placebo (N = 668) groups in controlled studies were compared with respect to (1) mean change from baseline in various ECG parameters, and (2) the incidence of patients meeting criteria for clinically significant changes from baseline in these variables.
No clinically meaningful changes in ECG parameters from baseline to final visit were observed for patients in controlled studies.
Other Reactions Observed During the Premarketing Evaluation of EMSAM
The following listing does not include reactions: 1) already listed elsewhere in labeling, 2) for which a causal relationship to drug was remote, 3) which were so general as to be uninformative, 4) which were not considered to have significant clinical implications, or 5) which occurred at a rate equal to or less than placebo.
Cardiovascular System: Tachycardia.
Digestive System: Anorexia.
Nervous System: Agitation, amnesia, tremor, twitching.
Skin and Appendages: Pruritus.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of EMSAM.
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Nervous System: Convulsion and hypoesthesia.
Psychiatric System: Disorientation, hallucination (visual), and tension.
Drug Interactions
There is limited information regarding Selegiline (transdermal) Drug Interactions in the drug label.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA):
There is no FDA guidance on usage of Selegiline (transdermal) in women who are pregnant.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Selegiline (transdermal) in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Selegiline (transdermal) during labor and delivery.
Nursing Mothers
There is no FDA guidance on the use of Selegiline (transdermal) in women who are nursing.
Pediatric Use
There is no FDA guidance on the use of Selegiline (transdermal) in pediatric settings.
Geriatic Use
There is no FDA guidance on the use of Selegiline (transdermal) in geriatric settings.
Gender
There is no FDA guidance on the use of Selegiline (transdermal) with respect to specific gender populations.
Race
There is no FDA guidance on the use of Selegiline (transdermal) with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Selegiline (transdermal) in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Selegiline (transdermal) in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Selegiline (transdermal) in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Selegiline (transdermal) in patients who are immunocompromised.
Administration and Monitoring
Administration
There is limited information regarding Selegiline (transdermal) Administration in the drug label.
Monitoring
There is limited information regarding Selegiline (transdermal) Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Selegiline (transdermal) and IV administrations.
Overdosage
10.1 Signs and Symptoms EMSAM overdosage may resemble overdosage with other nonselective, oral MAOI antidepressants and present with any of the following: drowsiness, dizziness, faintness, irritability, hyperactivity, agitation, severe headache, hallucinations, trismus, opisthotonos, convulsions, coma, rapid and irregular pulse, hypertension, hypotension and vascular collapse, precordial pain, respiratory depression and failure, hyperpyrexia, diaphoresis, and cool, clammy skin.
10.2 Management of Overdose There are no specific antidotes for EMSAM.
If symptoms of overdosage occur, immediately remove the EMSAM system and institute appropriate supportive therapy. For contemporary information on the management of poisoning or overdosage, contact the National Poison Control Center at 1-800-222-1222.
Delays of up to 12 hours between ingestion of drug and the appearance of signs may occur, and peak effects may not be observed for 24 to 48 hours. Since death has been reported following overdosage with MAOI agents, hospitalization with close monitoring during this period is strongly recommended.
In order to avoid the occurrence of hypertensive crisis (“cheese reaction”), dietary tyramine should be restricted for several weeks beyond recovery to permit regeneration of the peripheral MAO-A isoenzyme.
Pharmacology
There is limited information regarding Selegiline (transdermal) Pharmacology in the drug label.
Mechanism of Action
The mechanism of action of selegiline (the drug substance of EMSAM) as an antidepressant is not fully understood, but is presumed to be linked to potentiation of monoamine neurotransmitter activity in the central nervous system (CNS) resulting from its irreversible inhibition of the enzyme monoamine oxidase (MAO).
Structure
There is limited information regarding Selegiline (transdermal) Structure in the drug label.
Pharmacodynamics
MAO exists as two isoenzymes, referred to as MAO-A and MAO-B. Selegiline has a greater affinity for MAO-B, compared to MAO-A. However, at antidepressant doses, selegiline inhibits both isoenzymes. In an in vivo animal model used to test for antidepressant activity (Forced Swim Test), selegiline administered by transdermal system exhibited antidepressant properties only at doses that inhibited both MAO-A and MAO-B activity in the brain. In the CNS, MAO-A and MAO-B play important roles in the catabolism of neurotransmitter amines such as norepinephrine, dopamine, and serotonin, as well as neuromodulators such as phenylethylamine.
Receptor Binding
In in vitro receptor binding assays, selegiline has demonstrated affinity for the human recombinant adrenergic α2B receptor (Ki = 0.3 mcM). No affinity [Ki greater than 10 mcM] was noted at dopamine receptors, adrenergic β3, glutamate, muscarinic M1-M5, nicotinic, or rolipram receptor/sites.
Interaction with Tyramine
Selegiline (the drug substance of EMSAM) is an irreversible inhibitor of monoamine oxidase (MAO), a ubiquitous intracellular enzyme. MAO exists as two isoenzymes, referred to as MAO-A and MAO-B. Selegiline shows greater affinity for MAO-B; however, as selegiline concentration increases, this selectivity is lost with resulting dose-related inhibition of MAO-A. Intestinal MAO is predominantly type A, while in the brain both isoenzymes exist.
MAO plays a vital physiological role in terminating the biological activity of both endogenous and exogenous amines. In addition to their role in the catabolism of monoamines in the CNS, MAOs are also important in the catabolism of exogenous amines found in a variety of foods and drugs. MAO in the gastrointestinal tract (primarily type A) provides protection from exogenous amines with vasopressor actions, such as tyramine, which if absorbed intact can cause a hypertensive crisis, the so-called “cheese reaction”. If a large amount of tyramine is absorbed systemically, it is taken up by adrenergic neurons and causes norepinephrine release from neuronal storage sites with resultant elevation of blood pressure. While most foods contain negligible amounts or no tyramine, certain food products may contain large amounts of tyramine that represent a potential risk for hypertensive crisis [see WARNINGS AND PRECAUTIONS (5.3)].
To define the risk of hypertensive crises with use of EMSAM, several Phase I tyramine challenge studies were conducted both with and without food. Fourteen tyramine challenge studies including 214 healthy subjects (age range 18 to 65; 31 subjects greater than 50 years of age) were conducted to determine the pressor effects of oral tyramine with concurrent EMSAM treatment (6 mg per 24 hours to 12 mg per 24 hours), measured as the dose of tyramine required to raise systolic blood pressure by 30 mmHg (TYR30). Studies were conducted with and without concomitant administration of food. Studies conducted with food are most relevant to clinical practice since tyramine typically will be consumed in food. A high-tyramine meal is considered to contain up to 40 mg of tyramine.
One study using a crossover design in 13 subjects investigated tyramine pressor doses (TYR30) after administration of EMSAM 6 mg per 24 hours and oral selegiline (5 mg twice daily) for 9 days. Mean pressor doses (TYR30) of tyramine capsules administered without food were 338 mg and 385 mg in subjects treated with EMSAM and oral selegiline, respectively.
Another study using a crossover design in 10 subjects investigated tyramine pressor doses after administration of EMSAM 6 mg per 24 hours or tranylcypromine 30 mg per day for 10 days. Mean pressor doses (TYR30) of tyramine capsules administered without food were 270 mg in subjects treated with EMSAM 6 mg per 24 hours and 10 mg in subjects treated with tranylcypromine.
In a third crossover study, tyramine without food was administered to 12 subjects. The mean tyramine pressor doses (TYR30) after administration of EMSAM 6 mg per 24 hours for 9 and 33 days were 292 mg and 204 mg, respectively. The lowest pressor dose was 50 mg in one subject in the 33-day group.
Tyramine pressor doses were also studied in 11 subjects after extended treatment with EMSAM 12 mg per 24 hours. At 30, 60, and 90 days, the mean pressor doses (TYR30) of tyramine administered without food were 95 mg, 72 mg, and 88 mg, respectively. The lowest pressor dose without food was 25 mg in three subjects at day 30 while on EMSAM 12 mg per 24 hours. Eight subjects from this study, with a mean tyramine pressor dose of 64 mg at 90 days, were subsequently administered tyramine with food, resulting in a mean pressor dose of 172 mg (2.7 times the mean pressor dose observed without food, p less than 0.003).
With the exception of one study (N = 153), the Phase III clinical development program was conducted without requiring a modified diet (N = 2,553, 1,606 at 6 mg per 24 hours, and 947 at 9 mg per 24 hours or 12 mg per 24 hours). No hypertensive crises were reported in any patient receiving EMSAM.
Overall, the data for EMSAM 6 mg per 24 hours support a recommendation that a modified diet is not required at this dose. Due to the more limited data available for EMSAM 9 mg per 24 hours and the results from the Phase I tyramine challenge study in fed volunteers administered EMSAM 12 mg per 24 hours, patients receiving these doses should follow Dietary Modifications Required for Patients Taking EMSAM 9 mg per 24 hours and 12 mg per 24 hours [see WARNINGS AND PRECAUTIONS (5.3)].
Pharmacokinetics
There is limited information regarding Selegiline (transdermal) Pharmacokinetics in the drug label.
Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility Carcinogenesis
In a dermal carcinogenicity study in CD-1 mice, selegiline (the drug substance of EMSAM) was administered daily for 2 years at the same skin site at dose levels of 20, 70, and 200 mg per kg per day (dissolved in acetone). The incidence of systemic tumors was not increased and the high dose provided systemic exposures to selegiline and its three metabolites in mice that were greater than 40 times the exposures in humans at the maximum recommended human dose (MRHD). The incidence of squamous cell carcinoma was slightly increased on treated skin of mice administered the high dose. This finding was associated with an increased incidence of epithelial hyperplasia, dyskeratosis/hyperkeratosis and inflammation.
In an oral carcinogenicity study in rats, selegiline given in the diet for 104 weeks was not carcinogenic up to the highest evaluable dose tested (3.5 mg per kg per day), which exposed rats to systemic levels of selegiline and its three metabolites that were comparable to those in humans at the MRHD.
Mutagenesis
Selegiline induced mutations and chromosomal damage when tested in the in vitro mouse lymphoma assay with and without metabolic activation. Selegiline was negative in the Ames assay, the in vitro mammalian chromosome aberration assay in human lymphocytes, and the in vivo oral mouse micronucleus assay.
Impairment of Fertility
A mating and fertility study was conducted in male and female rats at transdermal doses of 10, 30, and 75 mg per kg per day of selegiline (8, 24, and 60 times the maximum recommended human dose of EMSAM [12 mg per 24 hours] on a mg per m2 basis). Slight decreases in sperm concentration and total sperm count were observed at the high dose; however, no significant adverse effects on fertility or reproductive performance were observed.
Clinical Studies
There is limited information regarding Selegiline (transdermal) Clinical Studies in the drug label.
How Supplied
There is limited information regarding Selegiline (transdermal) How Supplied in the drug label.
Storage
There is limited information regarding Selegiline (transdermal) Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Selegiline (transdermal) |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Selegiline (transdermal) |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Selegiline (transdermal) Patient Counseling Information in the drug label.
Precautions with Alcohol
Alcohol-Selegiline (transdermal) interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
There is limited information regarding Selegiline (transdermal) Brand Names in the drug label.
Look-Alike Drug Names
There is limited information regarding Selegiline (transdermal) Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.