Scleroderma case study one
|
Scleroderma Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Scleroderma case study one On the Web |
|
American Roentgen Ray Society Images of Scleroderma case study one |
|
Risk calculators and risk factors for Scleroderma case study one |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Case #1
Clinical Summary
A 29-year-old black female had a history of scleroderma involving the lung, kidney, heart, and skin. Her main clinical problems centered on her restrictive lung disease. She was able to live at home with supplemental oxygen but recently she had developed edema, chest pain, weakness, lightheadedness, and a loss of appetite. The patient was admitted to the hospital with a working diagnosis of congestive heart failure brought on by her lung disease.
Echocardiographic evaluation revealed a pericardial effusion that was tapped. Soon after this procedure her respiratory status degenerated and she required intubation. Despite aggressive supportive treatment for her cardiac and pulmonary problems, she could not be weaned from the ventilator. Two weeks after admission she became febrile and Gram positive cocci were isolated from sputum culture. She was placed on antibiotics but her condition deteriorated and she developed bradycardia followed by electromechanical dissociation (EMD).
Autopsy Findings
Upon opening the thorax there was 600 cc of cloudy serous fluid in each hemithorax and 100 cc of similar fluid in the pericardial sac. The heart weighed 530 grams and there was thickening of both the left and right ventricular walls. The liver weighed 1880 grams and was congested. The spleen weighed 200 grams and was also congested. The combined lung weight was 1875 grams; the lungs were markedly fibrotic with severe emphysema. In addition, dermal thickening was evident throughout the body and the wall of the esophagus was thickened and firm.
Histopathological Findings
-
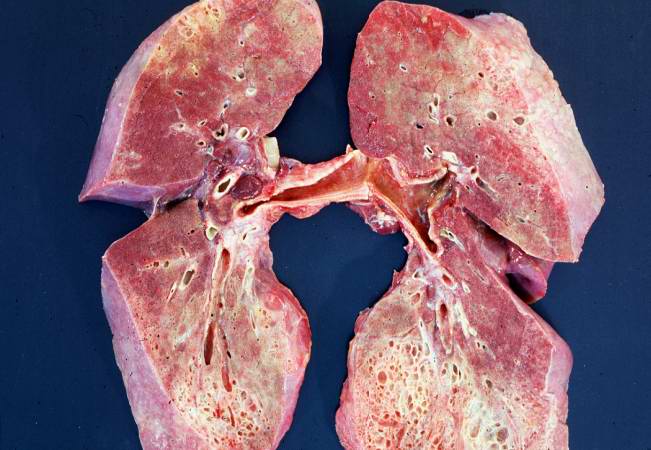
This is a gross photograph of cut section of the lungs from this patient. Note the extensive fibrosis of the lung parenchyma.
-
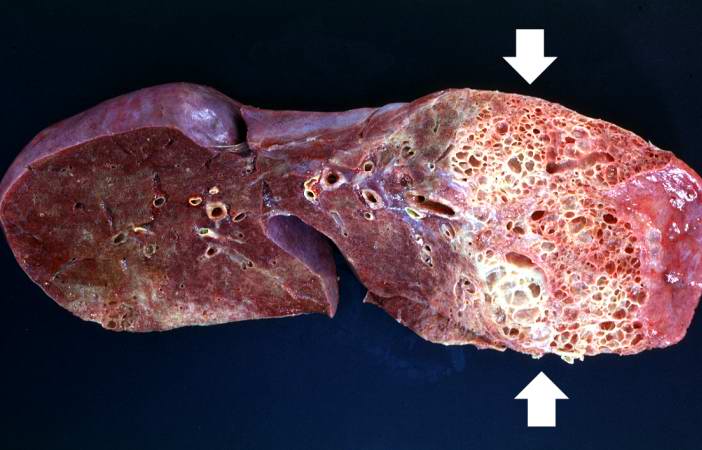
This is a gross photograph of a cut section of one lung from this patient. Note the extensive fibrosis lower lobe (arrows).
-
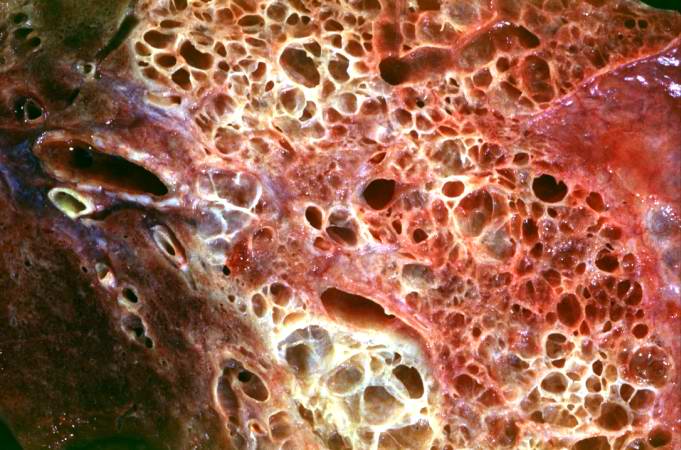
This is a closer view of the cut section of lung from this patient. Note the extensive fibrosis and the severe emphysematous changes.
-
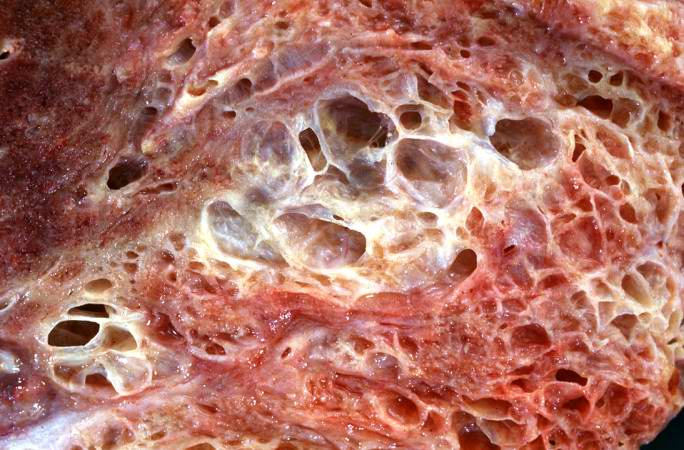
This is a closer view of the cut section of lung from this patient showing the extensive fibrosis and the severe emphysematous change.
-
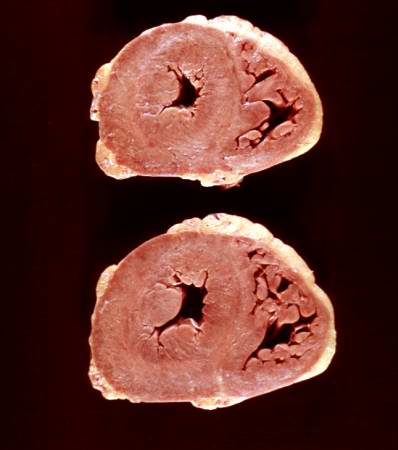
This is a gross photograph of the heart from this case. There is thickening of the left ventricular wall and some thickening of the right ventricle as well.
Sources
Images courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology [2]