Sandbox : anmol: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
No edit summary |
||
| Line 6: | Line 6: | ||
==Overview== | ==Overview== | ||
* [[Lyme disease]] is a condition commonly caused by bite of a tick infected with Borrelia burgdorferi. | * [[Lyme disease]] is a condition commonly caused by bite of a [[tick]] infected with [[Borrelia burgdorferi]]. | ||
==What are the symptoms of Lyme disease?== | ==What are the symptoms of Lyme disease?== | ||
{| | {| | ||
| | | | ||
* It's important to know the symptoms of Lyme disease and to seek medical help if you think have Lyme disease. | * It's important to know the symptoms of [[Lyme disease]] and to seek medical help if you think have [[Lyme disease]]. | ||
*Early signs and symptoms (3 to 30 days after tick bite): | *'''Early signs and symptoms (3 to 30 days after [[tick]] bite):''' | ||
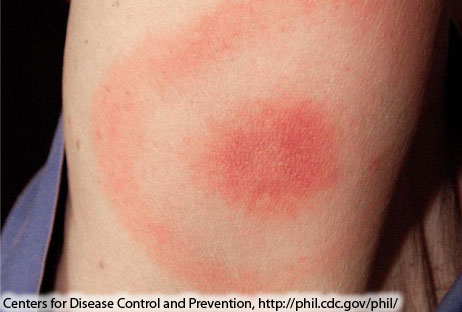
**The first symptom is usually a red rash at the site of tick bite, which may look like a bull's eye. But not all people with Lyme disease have a rash. The rash is called erythema chronicum migrans or erythema migrans (EM). | **The first symptom is usually a red rash at the site of [[tick]] bite, which may look like a bull's eye. But not all people with Lyme disease have a [[rash]]. The rash is called [[erythema chronicum migrans]] or [[erythema migrans]] (EM). | ||
***EM occurs in approximately 70 to 80 percent of infected persons. | ***EM occurs in approximately 70 to 80 percent of [[infected]] persons. | ||
***EM begins at the site of a tick bite after a delay of 3 to 30 days (average is about 7 days). | ***EM begins at the site of a [[tick]] bite after a delay of 3 to 30 days (average is about 7 days). | ||
***Em expands gradually over a period of days reaching up to 12 inches or more (30 cm) across. | ***Em expands gradually over a period of days reaching up to 12 inches or more (30 cm) across. | ||
***EM may feel warm to the touch but is rarely itchy or painful. | ***EM may feel warm to the touch but is rarely [[itchy]] or [[painful]]. | ||
***Sometimes, EM clears as it enlarges, resulting in a target or “bull’s-eye” appearance. | ***Sometimes, EM clears as it enlarges, resulting in a target or “bull’s-eye” appearance. | ||
***EM may appear on any area of the body but majority of times present in areas including axilla, inguinal region, popliteal fossa, or along belt line. | ***EM may appear on any area of the body but majority of times present in areas including [[axilla]], [[inguinal region]], [[popliteal fossa]], or along belt line. | ||
**The rash may or may not be associated with flu-like symptoms including: | **The rash may or may not be associated with flu-like symptoms including: | ||
***Fever and/or chills | ***[[Fever (patient information)|Fever]] and/or [[chills]] | ||
***Headache | ***[[Headache (patient information)|Headache]] | ||
***Body aches | ***[[Body aches]] | ||
***Joint aches | ***[[Arthralgia (patient information)|Joint aches]] | ||
***Headaches | ***[[Headache (patient information)|Headaches]] | ||
***Stiff neck | ***[[Neck stiffness/pain (patient information)|Stiff neck]] | ||
***Fatigue | ***[[Fatigue (patient information)|Fatigue]] | ||
| | | | ||
[[Image:Classic Lyme disease rash.jpg|thumb|250px|center|Classic Lyme disease rash - [https://www.cdc.gov/lyme/signs_symptoms/rashes.html Source: CDC.gov]]] | [[Image:Classic Lyme disease rash.jpg|thumb|250px|center|Classic Lyme disease rash - [https://www.cdc.gov/lyme/signs_symptoms/rashes.html Source: CDC.gov]]] | ||
|} | |} | ||
* | *Late Signs and Symptoms (days to months after tick bite): | ||
**Severe headaches and neck stiffness | **Severe [[Headache (patient information)|headaches]] and [[Neck stiffness/pain (patient information)|neck stiffness]] | ||
***Multiple | ***Multiple [[erythema migrans]] rashes on other areas of the body. | ||
***Arthritis with severe joint pain and swelling, particularly the knees and other large joints. | ***[[Arthritis (patient information)|Arthritis]] with severe [[Arthralgia (patient information)|joint pain]] and [[Swelling (medical)|swelling]], particularly the [[knees]] and other large joints. | ||
***Facial palsy (loss of muscle tone or droop on one or both sides of the face) | ***Facial palsy (loss of muscle tone or droop on one or both sides of the face). | ||
***Intermittent pain in tendons, muscles, joints, and bones | ***Intermittent pain in [[tendons]], [[muscles]], [[Joints (anatomy)|joints]], and bones. | ||
***Heart palpitations or an irregular heart beat (Lyme carditis) | ***[[Heart palpitations]] or an irregular [[heart beat]] ([[Lyme carditis]]). | ||
***Episodes of dizziness or shortness of breath | ***Episodes of [[Dizziness (patient information)|dizziness]] or [[Dyspnea (patient information)|shortness of breath]]. | ||
***Inflammation of the brain and spinal cord | ***[[Inflammation]] of the [[brain]] and [[spinal cord]]. | ||
***Nerve pain | ***[[Nerve pain]]. | ||
***Shooting pains, numbness, or tingling in the hands or feet | ***Shooting [[pains]], [[numbness]], or [[tingling]] in the [[hands]] or [[feet]]. | ||
***Problems with short-term memory | ***Problems with short-term [[memory]]. | ||
{| | {| | ||
| | | | ||
===Notes=== | ===Notes=== | ||
*Fever and other flu-like symptoms may occur in the absence of rash. | *[[Fever]] and other flu-like symptoms may occur in the absence of [[rash]]. | ||
*A small bump or redness at the site of a tick bite that occurs immediately and resembles a mosquito bite, is common. This irritation generally goes away in 1-2 days and is not a sign of Lyme disease. | *A small bump or redness at the site of a [[tick]] bite that occurs immediately and resembles a [[mosquito]] bite, is common. This irritation generally goes away in 1-2 days and is not a sign of [[Lyme disease]]. | ||
*A rash with a very similar appearance to EM occurs with Southern Tick-associated Rash Illness (STARI), but is not Lyme disease | *A [[rash]] with a very similar appearance to EM occurs with [[Southern tick-associated rash illness (patient information)|Southern Tick-associated Rash Illness]] (STARI), but is not Lyme disease. | ||
*Ticks can spread other organisms that may cause a different type of rash. | *[[Ticks]] can spread other organisms that may cause a different type of [[rash]]. | ||
==What causes Lyme disease?== | ==What causes Lyme disease?== | ||
* Lyme disease is caused by a bacterial infection you get from bite of an infected tick. | * [[Lyme disease]] is caused by a [[bacterial infection]] you get from bite of an infected [[tick]]. | ||
*The majority of Lyme disease in North America is caused by bite of black-legged tick, or deer tick(''[[Ixodes | *The majority of [[Lyme disease]] in North America is caused by bite of [[Ixodes scapularis|black-legged tick]], or [[deer tick]] (''[[Ixodes scapularis]]''). | ||
*Other ticks that transmit Lyme disease are [[Ixodes ricinus|sheep tick]], [[Ixodes ricinus|castor bean tick]], or [[Ixodes ricinus|European castor bean tick]] (''[[Ixodes ricinus]]'') in the Europe; [[Ixodes pacificus|Western black legged tick]] (''[[Ixodes pacificus]]'') in the Pacific region of North America; taiga tick (''Ixodes persulactus'') Europe, Central and Northern Asia, China, and Japan. | *Other ticks that transmit Lyme disease are [[Ixodes ricinus|sheep tick]], [[Ixodes ricinus|castor bean tick]], or [[Ixodes ricinus|European castor bean tick]] (''[[Ixodes ricinus]]'') in the Europe; [[Ixodes pacificus|Western black legged tick]] (''[[Ixodes pacificus]]'') in the Pacific region of North America; taiga tick (''Ixodes persulactus'') Europe, Central and Northern Asia, China, and Japan. | ||
*Only 20% of individuals [[Infection|infected]] with [[Lyme disease]] by the [[Ixodes scapularis|deer tick]] are aware of having had any [[tick]] bite. | *Only 20% of individuals [[Infection|infected]] with [[Lyme disease]] by the [[Ixodes scapularis|deer tick]] are aware of having had any [[tick]] bite. | ||
| Line 62: | Line 62: | ||
==Who is at highest risk?== | ==Who is at highest risk?== | ||
Individuals who spend time outdoors and/or have pets that go outdoors in [[Endemic (epidemiology)|endemic]] regions are at risk for [[tick-borne disease]]. | Individuals who spend time outdoors and/or have pets that go outdoors in [[Endemic (epidemiology)|endemic]] regions are at risk for [[tick-borne disease]]. | ||
===Exposure to ticks=== | ===Exposure to ticks=== | ||
*Individuals with frequent exposure to dogs and who reside near wooded areas or areas with high grass may also be at increased risk of [[tick-borne infection]]. | *Individuals with frequent exposure to dogs and who reside near wooded areas or areas with high grass may also be at increased risk of [[tick-borne infection]]. | ||
*Individuals with outdoor occupations and who work outside with bare or exposed [[skin]] are at a high risk of contracting Lyme disease. | *Individuals with outdoor occupations and who work outside with bare or exposed [[skin]] are at a high risk of contracting Lyme disease. | ||
*Failing to remove a [[tick]] as soon as you see it on your [[skin]] (the longer a [[tick]] is attached to your skin, the greater your risk of developing [[Lyme disease]]) also increases risk of developing Lyme disease. | *Failing to remove a [[tick]] as soon as you see it on your [[skin]] (the longer a [[tick]] is attached to your skin, the greater your risk of developing [[Lyme disease]]) also increases risk of developing Lyme disease. | ||
===Endemic Regions=== | ===Endemic Regions=== | ||
*About 95% of all reported cases are confined to 14 states including Connecticut, Delaware, Maine, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. | *About 95% of all reported cases are confined to 14 states including Connecticut, Delaware, Maine, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. | ||
*Any individual traveling or living within these five geographic areas including New England, Mid-Atlantic, East-North Central, South Atlantic, and West North-Central is at a heightened risk of exposure to [[Lyme disease]]. | *Any individual traveling or living within these five geographic areas including New England, Mid-Atlantic, East-North Central, South Atlantic, and West North-Central is at a heightened risk of exposure to [[Lyme disease]]. | ||
| Line 78: | Line 78: | ||
===Rarer forms of Transmission=== | ===Rarer forms of Transmission=== | ||
* Cases of [[blood transfusion]] and [[organ transplantation]] have been recorded as methods of [[Transmission (medicine)|transmission]] but this is a rare mode of transmission. | * Cases of [[blood transfusion]] and [[organ transplantation]] have been recorded as methods of [[Transmission (medicine)|transmission]] but this is a rare mode of transmission. | ||
==Diagnosis== | ==Diagnosis== | ||
*Following points should be taken into consideration in order to make a diagnosis of Lyme disease: | *Following points should be taken into consideration in order to make a diagnosis of [[Lyme disease]]: | ||
**A history of exposure to potentially infected ticks, especially in areas of the country known to have Lyme disease. | **A history of exposure to potentially infected [[ticks]], especially in areas of the country known to have [[Lyme disease]]. | ||
**Symptoms, including physical findings such as the characteristic rash. | **Symptoms, including physical findings such as the characteristic rash ([[erythema migrans]]). | ||
**Results of blood tests that check for antibodies to the bacterium that causes Lyme disease. | **Results of blood tests that check for [[antibodies]] to the [[bacterium]] that causes [[Lyme disease]]. | ||
==When to seek urgent medical care?== | ==When to seek urgent medical care?== | ||
*Lyme disease is rarely fatal. | *[[Lyme disease]] is rarely fatal. | ||
==Treatment options== | ==Treatment options== | ||
*According to CDC, patients treated with antibiotics in the early stages of the infection usually recover rapidly and completely. | *According to CDC, patients treated with [[antibiotics]] in the early stages of the infection usually recover rapidly and completely. | ||
*Antibiotics commonly used for oral treatment include doxycycline, amoxicillin, or cefuroxime axetil (Ceftin). | *Antibiotics commonly used for oral treatment include [[doxycycline]], [[amoxicillin]], or [[Cefuroxime axetil (oral)|cefuroxime axetil]] ([[Ceftin]]). | ||
*Patients with certain neurological or cardiac forms of illness may require intravenous treatment with drugs such as ceftriaxone or penicillin. | *Patients with certain [[neurological]] or [[cardiac]] forms of illness may require [[Intravenous therapy|intravenous]] treatment with drugs such as [[Ceftriaxone Sodium Injection (patient information)|ceftriaxone]] or [[penicillin]]. | ||
==Where to find medical care for Lyme disease?== | ==Where to find medical care for Lyme disease?== | ||
| Line 102: | Line 101: | ||
==Prevention== | ==Prevention== | ||
*Educate yourself about Lyme disease, and try not to get bitten by ticks. More specifically: | *Educate yourself about [[Lyme disease]], and try not to get bitten by ticks. | ||
*Avoid wooded, brushy, and grassy areas, especially in May, June, and July. (Contact the local health department or park/extension service for information on the prevalence of ticks in specific areas.) | *More specifically: | ||
*Wear light-colored clothing so that you can see ticks that get on you. | **Avoid wooded, brushy, and grassy areas, especially in May, June, and July. (Contact the local health department or park/extension service for information on the [[prevalence]] of [[Tick|ticks]] in specific areas.) | ||
*Wear long pants and long-sleeved shirts. | **Wear light-colored clothing so that you can see ticks that get on you. | ||
*Wear shoes that cover the entire foot. Tuck pant legs into socks or shoes, and tuck shirts into pants. | **Wear long pants and long-sleeved shirts. | ||
*Wear a hat for extra protection. | **Wear shoes that cover the entire foot. Tuck pant legs into socks or shoes, and tuck shirts into pants. | ||
*Spray insect repellent containing DEET on clothes and exposed skin other than the face, or treat clothes with permethrin, which kills ticks on contact. | **Wear a hat for extra protection. | ||
*Walk in the center of trails to avoid brush and grass. | **Spray insect repellent containing [[DEET]] on clothes and exposed skin other than the face, or treat clothes with [[Permethrin (patient information)|permethrin]], which kills [[ticks]] on contact. | ||
*Remove your clothing, and wash and dry them at high temperatures after being outdoors. | **Walk in the center of trails to avoid brush and grass. | ||
*Do a careful body check for ticks after outdoor activities. | **Remove your clothing, and wash and dry them at high temperatures after being outdoors. | ||
**Do a careful body check for ticks after outdoor activities. | |||
*If a tick is attached to you, remove it! | *If a tick is attached to you, remove it! | ||
**Using tweezers, grasp the tick close to the skin, pull straight back, and avoid crushing the tick's body. | **Using tweezers, grasp the [[tick]] close to the skin, pull straight back, and avoid crushing the tick's body. | ||
**Save the tick for possible identification by a doctor or the local health department. | **Save the [[tick]] for possible identification by a doctor or the local health department. | ||
==What to expect (Outlook/Prognosis)?== | ==What to expect (Outlook/Prognosis)?== | ||
| Line 121: | Line 121: | ||
**Late diagnosis | **Late diagnosis | ||
**Failure of antibiotic treatment | **Failure of antibiotic treatment | ||
**Coinfection with other tick-borne diseases including Ehrlichiosis and Babesiosis | **Coinfection with other tick-borne diseases including [[Ehrlichiosis (patient information)|Ehrlichiosis]] and [[Babesiosis (patient information)|Babesiosis]] | ||
**Immune suppression in the patient | **[[Immune suppression]] in the patient | ||
*Some patients with Lyme disease have fatigue, joint and/or muscle pain, and neurocognitive symptoms persisting for years despite antibiotic treatment. | *Some patients with [[Lyme disease]] have [[Fatigue (patient information)|fatigue]], [[Arthralgia (patient information)|joint]] and/or [[Myalgia (patient information)|muscle pain]], and [[neurocognitive]] symptoms persisting for years despite [[antibiotic]] treatment. | ||
*Patients with late stage Lyme disease have been shown to experience a level of physical disability similar to that seen in congestive heart failure. | *Patients with late stage [[Lyme disease]] have been shown to experience a level of physical disability similar to that seen in [[Congestive heart failure (patient information)|congestive heart failure]]. | ||
*Though rare, Lyme disease can be fatal. | *Though rare, [[Lyme disease]] can be fatal. | ||
==Possible complications== | ==Possible complications== | ||
*Late Lyme disease can cause long-term joint inflammation (Lyme arthritis) and heart rhythm problems. Brain and nervous system problems are also possible, and may include: | *Late [[Lyme disease]] can cause long-term [[Joint (anatomy)|joint]] [[inflammation]] ([[Lyme arthritis]]) and [[heart rhythm]] problems. [[Brain]] and [[nervous system]] problems are also possible, and may include: | ||
**Decreased concentration | **Decreased concentration | ||
**Memory disturbances | **Memory disturbances | ||
**Nerve damage | **[[Nerve damage]] | ||
**Numbness | **[[Numbness]] | ||
**Pain | **[[Pain(patient information)|Pain]] | ||
**Paralysis of the face muscles | **[[Paralysis]] of the face muscles | ||
**Sleep disorders | **Sleep disorders | ||
**Vision problems | **Vision problems | ||
| Line 142: | Line 142: | ||
* https://www.cdc.gov/lyme/index.html | * https://www.cdc.gov/lyme/index.html | ||
* https://www.fda.gov/ForConsumers/ConsumerUpdates/ucm049298.htm | * https://www.fda.gov/ForConsumers/ConsumerUpdates/ucm049298.htm | ||
[[Category:Help]] | [[Category:Help]] | ||
Revision as of 16:58, 7 August 2017
To go back to Lyme disease main page, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Anmol Pitliya, M.B.B.S. M.D.[2]
Overview
- Lyme disease is a condition commonly caused by bite of a tick infected with Borrelia burgdorferi.
What are the symptoms of Lyme disease?
|
 |
- Late Signs and Symptoms (days to months after tick bite):
- Severe headaches and neck stiffness
- Multiple erythema migrans rashes on other areas of the body.
- Arthritis with severe joint pain and swelling, particularly the knees and other large joints.
- Facial palsy (loss of muscle tone or droop on one or both sides of the face).
- Intermittent pain in tendons, muscles, joints, and bones.
- Heart palpitations or an irregular heart beat (Lyme carditis).
- Episodes of dizziness or shortness of breath.
- Inflammation of the brain and spinal cord.
- Nerve pain.
- Shooting pains, numbness, or tingling in the hands or feet.
- Problems with short-term memory.
- Severe headaches and neck stiffness
Notes
What causes Lyme disease?
|
 |
Who is at highest risk?
Individuals who spend time outdoors and/or have pets that go outdoors in endemic regions are at risk for tick-borne disease.
Exposure to ticks
- Individuals with frequent exposure to dogs and who reside near wooded areas or areas with high grass may also be at increased risk of tick-borne infection.
- Individuals with outdoor occupations and who work outside with bare or exposed skin are at a high risk of contracting Lyme disease.
- Failing to remove a tick as soon as you see it on your skin (the longer a tick is attached to your skin, the greater your risk of developing Lyme disease) also increases risk of developing Lyme disease.
Endemic Regions
- About 95% of all reported cases are confined to 14 states including Connecticut, Delaware, Maine, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin.
- Any individual traveling or living within these five geographic areas including New England, Mid-Atlantic, East-North Central, South Atlantic, and West North-Central is at a heightened risk of exposure to Lyme disease.
Seasonal Variation
- The majority of Lyme disease cases are reported during the summer months of May to August.
- Case incidence increases in May, peaks in June and July, and tapers off in August.
Rarer forms of Transmission
- Cases of blood transfusion and organ transplantation have been recorded as methods of transmission but this is a rare mode of transmission.
Diagnosis
- Following points should be taken into consideration in order to make a diagnosis of Lyme disease:
- A history of exposure to potentially infected ticks, especially in areas of the country known to have Lyme disease.
- Symptoms, including physical findings such as the characteristic rash (erythema migrans).
- Results of blood tests that check for antibodies to the bacterium that causes Lyme disease.
When to seek urgent medical care?
- Lyme disease is rarely fatal.
Treatment options
- According to CDC, patients treated with antibiotics in the early stages of the infection usually recover rapidly and completely.
- Antibiotics commonly used for oral treatment include doxycycline, amoxicillin, or cefuroxime axetil (Ceftin).
- Patients with certain neurological or cardiac forms of illness may require intravenous treatment with drugs such as ceftriaxone or penicillin.
Where to find medical care for Lyme disease?
- In this section you can provide links for reputable places that the patient can find good treatment for there condition.
Prevention
- Educate yourself about Lyme disease, and try not to get bitten by ticks.
- More specifically:
- Avoid wooded, brushy, and grassy areas, especially in May, June, and July. (Contact the local health department or park/extension service for information on the prevalence of ticks in specific areas.)
- Wear light-colored clothing so that you can see ticks that get on you.
- Wear long pants and long-sleeved shirts.
- Wear shoes that cover the entire foot. Tuck pant legs into socks or shoes, and tuck shirts into pants.
- Wear a hat for extra protection.
- Spray insect repellent containing DEET on clothes and exposed skin other than the face, or treat clothes with permethrin, which kills ticks on contact.
- Walk in the center of trails to avoid brush and grass.
- Remove your clothing, and wash and dry them at high temperatures after being outdoors.
- Do a careful body check for ticks after outdoor activities.
- If a tick is attached to you, remove it!
What to expect (Outlook/Prognosis)?
- For early cases, prompt treatment is usually curative.
- However, the severity and treatment of Lyme disease may be complicated due to:
- Late diagnosis
- Failure of antibiotic treatment
- Coinfection with other tick-borne diseases including Ehrlichiosis and Babesiosis
- Immune suppression in the patient
- Some patients with Lyme disease have fatigue, joint and/or muscle pain, and neurocognitive symptoms persisting for years despite antibiotic treatment.
- Patients with late stage Lyme disease have been shown to experience a level of physical disability similar to that seen in congestive heart failure.
- Though rare, Lyme disease can be fatal.
Possible complications
- Late Lyme disease can cause long-term joint inflammation (Lyme arthritis) and heart rhythm problems. Brain and nervous system problems are also possible, and may include:
- Decreased concentration
- Memory disturbances
- Nerve damage
- Numbness
- Pain
- Paralysis of the face muscles
- Sleep disorders
- Vision problems