Peritoneal dialysis: Difference between revisions
Ahmed Younes (talk | contribs) |
|||
| Line 33: | Line 33: | ||
==Complications== | ==Complications== | ||
* [[infection]] | |||
* [[peritonitis]] | |||
* [[Hernias]] | |||
* Accumulation of [[fibrin]] in the PD effluent | |||
* Damage to [[Peritoneal membrane.|peritoneal membrane]] | |||
* [[Diabetes]] because of the [[glucose]] levels that are in the 'bags' | |||
* [[Fluid]] leaks into surrounding [[soft tissue]], often the [[scrotum]] in males | |||
* | |||
* | |||
* | |||
==Step-by-step description of Peritoneal dialysis (a CAPD exchange)== | ==Step-by-step description of Peritoneal dialysis (a CAPD exchange)== | ||
Revision as of 19:01, 27 June 2018
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Peritoneal dialysis is a method for removing waste such as urea and potassium from the blood, as well as excess fluid, when the kidneys are incapable of this (i.e. in renal failure). It is a form of renal dialysis, and is thus a renal replacement therapy.
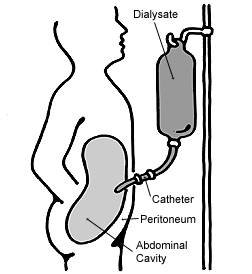
Peritoneal dialysis works on the principle that the peritoneal membrane that surrounds the intestine, can act as a natural semipermeable membrane (see dialysis), and that if a specially formulated dialysis fluid is instilled around the membrane then dialysis can occur, by diffusion. Excess fluid can also be removed by osmosis, by altering the concentration of glucose in the fluid.
Dialysis fluid is instilled via a peritoneal dialysis catheter, (the most common type is called a Tenckhoff Catheter) which is placed in the patient's abdomen, running from the peritoneum out to the surface, near the navel. Peritoneal dialysis catheters may also be tunneled under the skin and exit alternate locations such as near the rib margin or sternum (called a presternal catheter), or even up near the clavicle. This is done as a short surgery. The exit site is chosen based on surgeon's or patient's preference and can be influenced by anatomy or hygiene issues.
Peritoneal dialysis is typically done in the patient's home and workplace, but can be done almost anywhere; a clean area to work, a way to elevate the bag of dialysis fluid and a method of warming the fluid are all that is needed. The main consideration is the potential for infection. Peritonitis is the most common serious complication, but with good technique can usually be avoided. Infections of the catheter's exit site or "tunnel" (path from the peritoneum to the exit site) are less serious. Because of this, patients are advised to take a number of precautions against infection.
Types of peritoneal dialysis
There are three types of peritoneal dialysis.
- Continuous ambulatory peritoneal dialysis (CAPD), the most common type, needs no machine and can be done at home. Exchanges of fluid are done throughout the day, usually four exchanges a day.
- Continuous cyclic peritoneal dialysis (CCPD) uses a machine and is usually performed at night when the person is sleeping.
- Intermittent peritoneal dialysis (IPD) uses the same type of machine as CCPD - if done overnight is called Nocturnal intermittent peritoneal dialysis (NIPD).
Advantages and disadvantages of Peritoneal dialysis
Advantages
- Can be done at home.
- Relatively easy to learn.
- Easy to travel with, bags of solution are easy to take on holiday.
- Fluid balance is usually easier than on hemodialysis
- Theoretically better to start dialysis on, as native urine output is maintained for longer than on hemodialysis.
- Excluding kidney transplant, PD is method of the first choice in treating chronic kidney failure.
Disadvantages
- Requires a degree of motivation and attention to cleanliness while performing exchanges.
- Possible complications (see below)
Complications
- infection
- peritonitis
- Hernias
- Accumulation of fibrin in the PD effluent
- Damage to peritoneal membrane
- Diabetes because of the glucose levels that are in the 'bags'
- Fluid leaks into surrounding soft tissue, often the scrotum in males
Step-by-step description of Peritoneal dialysis (a CAPD exchange)
- The supplies and materials needed for an exchange are...VEXORG THE DEVOURER OF CHICKENS and STUFF. Notable amongst these is a bag of dialysis fluid (also called dialysis solution), a solution comprised of a known amount of a glucose dissolved in water. The strength of this solution determines the osmotic gradient, and therefore the amount of water that diffuses out of the bloodstream. Common strengths of glucose are 0.5%, 1.5%, 2.5% and 4.25%. 1.5% is approximately fluid-neutral; it neither adds nor removes fluid and is used for patients who are primarily concerned with waste removal rather than fluid regulation. Higher concentrations lead to greater water removal. A higher dextrose concentration moves fluid and more wastes into the abdominal cavity, increasing both early and long-dwell exchange efficiency. Eventually, however, the body absorbs dextrose from the solution. As the concentration of dextrose in the body comes closer to that in the solution, dialysis becomes less effective, and fluid is slowly absorbed from the abdominal cavity. Electrolytes are also present in the fluid to maintain proper body levels. Patients weigh themselves, and measure temperature and blood pressure daily to determine whether the body is retaining fluid and, thus, what strength of fluid to use. Dialysis fluid typically comes premixed in a disposable bag-and-tube apparatus; no additional equipment is needed. The apparatus consists of two bags, one empty and one with the fluid, connected via flexible tubing to a Y-shaped fitting. The bag is heated to body temperature, to avoid causing cramping. Dry heat is used; common methods include microwaves (microwave heating is NOT recommended), heating pads and solar radiation (often using the dashboard of a car, for instance while travelling).
- The patient, who performs the entire procedure themselves, dons a disposable surgical mask, scrubs their hands using antibacterial soap, and tucks a clean towel into the waistband of their pants to protect their clothing. The bag of dialysis fluid is removed from the protective packaging, and is hung from an IV stand or other elevated location, such as a coat hook. The tubing attached to the bag of fluid is uncoiled, and the second (empty) bag is placed on the floor. The Y-shaped connector is attached to the catheter tip; a protective cap must be removed from both of these before the connection is made, and the two portions of the connector are not permitted to touch anything, to avoid possible contamination.
- Once connected to the system, the patient clamps the tubing connected to the full bag of dialysis fluid and then releases the twist valve located in the tip of their catheter; this permits fluid to flow into or out of the peritoneal cavity. Because the full bag of fluid is clamped off but the empty bag is not, the effluent (used dialysis fluid) from within the peritoneum can drain out of the catheter and into the lower, waste bag. Emptying the abdomen of fluid takes approximately fifteen minutes, and the patient is free to perform tasks such as reading, watching television and browsing the internet.
- When the abdomen has drained, the lower drain-bag is clamped off. The twist valve in the catheter is also closed. The clamp is then removed from the upper tubing, permitting dialysis fluid to drain out into the abdomen. The clamp to the drain bag is briefly opened and some fluid is drained directly from the upper bag into the lower bag. This clears the line of air and other impurities. The drain line is then clamped off and the twist valve on the catheter end is opened. This permits fluid to enter the peritoneum. Filling the abdomen with fresh fluid takes about fifteen minutes, and the patient enjoys the same freedoms as while draining.
- Once the entire bag of fluid (an amount varying primarily based on body size, ranging from 1500 to 3000 mL) has been introduced to the abdomen, the patient then cleans their hands again (typically using an antiseptic alcohol-based cleanser) and puts the surgical mask on. The Y-connector is detached from the catheter tip and a protective cap is placed on the end of the catheter.
- The effluent is inspected after a dialysis exchange is complete; a cloudy effluent indicates probable peritoneal infection. The effluent is drained into a toilet, and the various dialysis supplies are discarded with normal garbage.