Palatine tonsil
Overview
Palatine tonsils are the tonsils that can be seen in the back of the throat.
Tonsillitis is an inflammation of the tonsils and will often, but not necessarily, cause a sore throat and fever. In chronic cases tonsillectomy may be indicated.[1]
Functions of palatine tonsils
Local immunity
Tonsillar (relating to palatine tonsil) B cells can mature to produce all the five major Ig classes. Furthermore, when incubated in vitro with either mitogens or specific antigens, they produce specific antibodies against diphtheria toxoid, poliovirus, Streptococcus pneumoniae, Haemophilus influenzae, Staphylococcus aureus, and the lipopolysaccharide of E. Most Immunoglobulin A produced by tonsillar B cells in vitro appears to be 7S monomers, although a significant proportion may be l0S dimeric IgA.
In addition to humoral immunity elicited by tonsillar and adenoidal B cells following antigenic stimulation, there is considerable T-cell response in palatine tonsils. Thus, natural infection or intranasal immunization with live, attenuated rubella virus vaccine has been reported to prime tonsillar lymphocytes much better than subcutaneous vaccination. Also, natural infection with varicella zoster virus has been found to stimulate tonsillar lymphocytes better than lymphocytes from peripheral blood.
Combined tonsillectomy and adenoidectomy had a profound detrimental effect on the local IgA response in the nasopharyngeal fluid against poliovirus. These immunological observations paralleled the increased incidence of paralytic poliomyelitis after this operation. Thus, it is obvious that the tonsil have an important role to play in the defense of the host against bacterial and viral infections, and the success of regional mucosal immunity induced by intranasal vaccines most likely depends on these immunocompetent tissues in the oropharynx and nasopharynx.
Altogether, therefore, several pieces of direct and indirect evidence indicate that the palatine tonsils are continuously engaged in local immune responses to microorganisms. If the tonsillar lymphocytes became overwhelmed with this persistent stimulation they may be unable to respond to other antigens; the immunological response, particularly in recurrent tonsillitis, may then be impaired. Once this immunological impairment occurs, the tonsil is no longer able to function adequately in local protection nor can it appropriately reinforce the secretory immune system of the upper respiratory tract.
Cytokine action
Cytokines are humoral immunomodulatory proteins or glycoproteins which control or modulate the activities of target cells, resulting in gene activation, leading to mitotic division, growth and differentiation, migration, or apoptosis. They are produced by wide range of cell types upon antigen-specific and non-antigen specific stimuli. It has been reported by many studies that the clinic outcome of many infectious, autoimmune, or malignant diseases appears to be influenced by the overall balance of production (profiles) of pro-inflammatory and anti-inflammatory cytokines. Therefore, determination of cytokine profiles in tonsil study will provide key information for further in-depth analysis of the cause and underlying mechanisms of these disorders, as well as the role and possible interactions between the T- and B-lymphocytes and other immunocompetent cells.
The cytokine network represents a very sophisticated and versatile regulatory system that is essential to the immune system for overcoming the various defense strategies of microorganisms. In our findings, the Th1 and Th2 cytokines and cytokine mRNA are both detectable in Tonsillar Hypertrophy and Recurrent Tonsillitis groups. It showed that human palatine tonsil is an active immunological organ containing a wide range of cytokine producing cells. Both Th1 and Th2 cells are involved in the pathophysiology of TH and RT conditions. Indeed, human tonsils persistently harbor microbial antigens even when the subject is asymptomatic of ongoing infection. It could also be an effect of ontogeny of the immune system.
Anatomy
The palatine tonsil is one of the mucosa-associated lymphoid tissues (MALT), located at the entrance to the upper respiratory and gastrointestinal tracts to protect the body from the entry of exogenous material through mucosal sites. In consequence it is a site of, and potential focus for infections, and is one of the chief immunocompetent tissues in the oropharynx. It forms part of the Waldeyer's ring, which comprises the nasopharyngeal tonsil or adenoid (NT), the paired tubal tonsils (TT), the paired palatine tonsils (PT) and the lingual tonsil (LT).
In children, the tonsils are common sites of infections that may give rise to acute or chronic tonsillitis. However, it is still an open question whether tonsillar hypertrophy is also caused by a persistent infection. Tonsillectomy is one of the most common major operations performed on children in Singapore. The indications for the operation have been complicated by the controversy over the benefits of removing a chronically infected tissue and the possible harm caused by eliminating an important immune inductive tissue.
The information that is necessary to make a rational decision to resolve this controversy can be obtained by understanding the immunological potential of the normal palatine tonsils and comparing these functions with the changes that occur in the chronically diseased counterparts.
Tonsilar crypts

Palatine tonsils consist of an extensive system of crypts generating a large internal surface. And the tonsils contain four lymphoid compartments participating in the immune functions, namely the reticular crypt epithelium, the extrafollicular area, the mantle zones of lymphoid follicles, and the follicular germinal centers. In human palatine tonsils, the very first part exposed to the outside environment is tonsillar epithelium.
The human palatine tonsils (PT) are covered by stratified squamous epithelium that extends into deep and partly branched crypts, of which there are about 10 to 30. The crypts greatly increase the contact surface between environmental influences and lymphoid tissue. In an average adult palatine tonsil the estimated epithelial surface area of the crypts is 295 cm2, in addition to the 45 cm2 of epithelium covering the oropharyngeal surface.
The crypts extend through the full thickness of the tonsil reaching almost to its hemicapsule. In healthy tonsils the openings of the crypts are fissure-like, and the walls of the lumina are in apposition. A computerized three-dimensional reconstruction of the palatine tonsil crypt system showed that in the centre of the palatine tonsil are tightly packed ramified crypts that join with each other, while on the periphery there is a rather simple and sparse arrangement.
The crypt system is not merely a group of invaginations of the tonsillar epithelium but a highly complicated network of canals with special types of epithelium and with various structures surrounding the canals, such as blood and lymphatic vessels and germinal centers.
Macrophages and other white blood cells concentrate by the tonsilar crypts as well, in response to the microorganisms attracted to the crypts. Accordingly, the tonsilar crypts serve a forward sentry role for the immune system, by providing early exposure of immune system cells to infectious organisms which may be introduced into the body via food or other ingested matter.
However, the tonsilar crypts often provide such an inviting environment to bacteria that bacterial colonies may form solidified "plugs" or "stones" within the crypts. In particular, sufferers of chronic sinusitis or post-nasal drip frequently suffer from these overgrowths of bacteria in the tonsilar crypts. These small whitish plugs, termed "tonsilloliths" and sometimes known as "tonsil stones," have a foul smell and can contribute to bad breath; furthermore, they can obstruct the normal flow of pus from the crypts, and may irritate the throat (people with tonsil stones may complain of the feeling that something is stuck in their throat).
Diseases
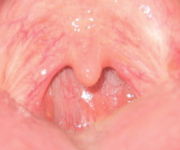
The pathogenesis of infectious/inflammatory disease in the tonsils most likely has its basis in their anatomic location and their inherent function as organ of immunity, processing infectious material, and other antigens and then becoming, ironically, a focus of infection/inflammation. No single theory of pathogenesis has yet been accepted, however. Viral infection with secondary bacterial invasion may be one mechanism of the initiation of chronic disease, but the effects of the environment, host factors, the widespread use of antibiotics, ecological considerations, and diet all may play a role.
Acute tonsillitis
Tonsillitis is the inflammation of tonsils. Acute tonsillitis is the most common manifestation of tonsillar disease. It is associated with sore throat, fever, and dysphagia. The tonsils may appear normal sized or enlarged but are usually erythematous. Often, but not always, exudates can be seen. Not all these signs and symptoms are present in every patient.
Recurrent tonsillitis
Recurrent infection has been variably defined as from four to seven episodes of acute tonsillitis in one year, five episodes for two consecutive years or three episodes per year for 3 consecutive years.
Tonsillar hypertrophy
Tonsillar hypertrophy is the enlargement of the tonsils, but without the history of inflammation. Obstructive tonsillar hypertrophy is currently the most common reason for tonsillectomy. These patients present with varying degrees of obstructive sleep and awake disturbances, which may include symptoms of loud snoring (accompanied by periods of irregular breathing), nocturnal choking and coughing, frequent awakenings with restless sleep, dysphagia, daytime hypersomnolence, and behavioral changes.
Additional images
-
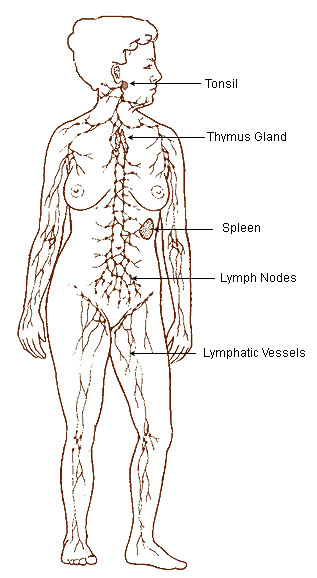
Lymphatic system
-
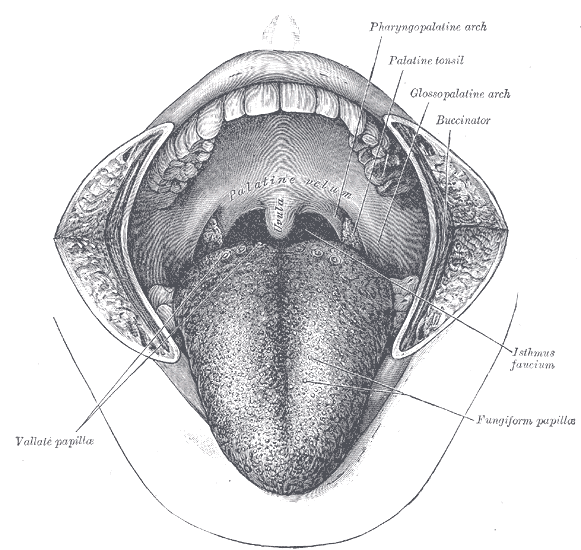
The mouth cavity. The cheeks have been slit transversely and the tongue pulled forward.
Footnotes
- ↑ Weil-Olivier C, Sterkers G, François M, Garnier J, Reinert P, Cohen R (2006). "[Tonsillectomy in 2005]". Arch Pediatr. 13 (2): 168–74. PMID 16386410.
External links
Template:Lymphatics of head and neck