Herpes simplex ocular infection: Difference between revisions
No edit summary |
m (Bot: Removing from Primary care) |
||
| (8 intermediate revisions by 4 users not shown) | |||
| Line 7: | Line 7: | ||
{{Herpes simplex}} | {{Herpes simplex}} | ||
{{CMG}} | {{CMG}}; '''Associate Editor-In-Chief:''' {{CZ}} | ||
==Overview== | ==Overview== | ||
Ocular herpes is generally caused by HSV-1 and is a special case of facial herpes infection known as herpes keratitis. It begins with infection of epithelial cells on the surface of the eye and retrograde infection of nerves serving the [[cornea]].<ref name="pmid11393165">{{cite journal |author=Carr DJ, Härle P, Gebhardt BM |title=The immune response to ocular herpes simplex virus type 1 infection |journal=Exp. Biol. Med. (Maywood) |volume=226 |issue=5 |pages=353–66 |year=2001 |pmid=11393165 |doi=}}</ref> | Ocular herpes is generally caused by [[HSV-1]] and is a special case of facial herpes infection known as herpes keratitis. It begins with infection of [[epithelial cells]] on the surface of the eye and [[retrograde infection]] of [[nerves]] serving the [[cornea]].<ref name="pmid11393165">{{cite journal |author=Carr DJ, Härle P, Gebhardt BM |title=The immune response to ocular herpes simplex virus type 1 infection |journal=Exp. Biol. Med. (Maywood) |volume=226 |issue=5 |pages=353–66 |year=2001 |pmid=11393165 |doi=}}</ref> | ||
==Diagnosis== | |||
== | ===History and Symptoms=== | ||
Primary infection typically presents as swelling of the [[conjunctiva]] and | Primary infection typically presents as [[swelling]] of the [[conjunctiva]] and eyelids ([[blepharoconjunctivitis]]), accompanied by small white itchy [[lesions]] on the surface of the [[cornea]], which vary from minor damage to the [[epithelium]] (superficial punctate keratitis) to the formation of [[Corneal ulcer|dendritic ulcers]].<ref name="pmid10858770">{{cite journal |author=Suresh PS, Tullo AB |title=Herpes simplex keratitis |journal=Indian J Ophthalmol |volume=47 |issue=3 |pages=155–65 |year=1999 |pmid=10858770 |doi=}}</ref> Infection is unilateral, affecting one eye at a time. Additional symptoms include dull pain deep inside the eye, mild to acute dryness, and [[sinusitis]]. Most primary infections resolve spontaneously in a few weeks or with the use of oral and topical [[antiviral]]s. However, the [[virus]] continues to inhabit the [[neurons]] of the eye and to multiply. | ||
Subsequent recurrences may be more severe, with infected [[epithelial cells]] showing larger [[Dendritic ulcer|dendritic ulceration]] and [[lesions]] forming white [[plaques]].<ref name="pmid10858770"/> The epithelial layer is sloughed off as the [[dendritic ulcer]] grows and mild [[inflammation]] ([[iritis]]) may occur in the underlying [[stroma of iris]]. Sensation loss occurs in lesional areas produces generalized corneal anaesthesia with repeated recurrences.<ref name="pmid10858770"/> This may be accompanied by chronic [[dry eye]], low-grade intermittent [[conjunctivitis]], or chronic unexplained [[sinusitis]]. When the concentration of viral DNA reaches a critical limit, the presence of the virus can trigger a massive [[autoimmune]] response in the eye, resulting in an individual's immune system destroying the [[Substantia propria|corneal stroma]].<ref name="pmid10858770"/> This usually results in [[Vision loss|loss of vision]] due to opacification of the [[cornea]] and is a result of an [[Antibody responses|antibody response]] against the [[viral]] [[antigen]] expression in the [[stroma]] following persistent infection.<ref name="pmid10858770"/> This is known as immune-mediated stromal keratitis. | |||
==Treatment== | ==Treatment== | ||
Treatment with corneal transplants was once ineffective (with | ===Surgery=== | ||
Treatment with [[Corneal transplant|corneal transplants]] was once ineffective (with a 14-61% rate of survival without antiviral therapy), as reinfection of the transplant is common when the [[virus]] reactivates. However, with concurrent use of antivirals the chance of graft acceptance has improved.<ref name="pmid12034687">{{cite journal |author=Halberstadt M, Machens M, Gahlenbek KA, Böhnke M, Garweg JG |title=The outcome of corneal grafting in patients with stromal keratitis of herpetic and non-herpetic origin |journal=Br J Ophthalmol |volume=86 |issue=6 |pages=646–52 |year=2002 |pmid=12034687 |doi=}}</ref> | |||
==References== | ==References== | ||
{{reflist|2}} | {{reflist|2}} | ||
{{WH}} | |||
{{WS}} | |||
[[Category:Sexually transmitted diseases]] | |||
[[Category:Viral diseases]] | |||
[[Category:Gynecology]] | |||
[[Category:Dermatology]] | |||
[[Category:Obstetrics]] | |||
[[Category:Disease]] | [[Category:Disease]] | ||
[[Category:Emergency mdicine]] | |||
[[Category:Up-To-Date]] | |||
[[Category:Infectious disease]] | [[Category:Infectious disease]] | ||
[[Category: | [[Category:Otolaryngology]] | ||
[[Category:Urology]] | |||
Latest revision as of 22:09, 29 July 2020
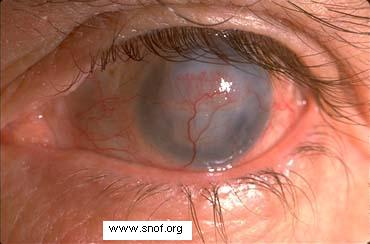
| Herpesviral ocular disease | |
 | |
|---|---|
| Herpes infection of the cornea |
|
Herpes simplex Microchapters |
|
Patient Information |
|
Classification |
|
Herpes simplex ocular infection On the Web |
|
Risk calculators and risk factors for Herpes simplex ocular infection |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Overview
Ocular herpes is generally caused by HSV-1 and is a special case of facial herpes infection known as herpes keratitis. It begins with infection of epithelial cells on the surface of the eye and retrograde infection of nerves serving the cornea.[1]
Diagnosis
History and Symptoms
Primary infection typically presents as swelling of the conjunctiva and eyelids (blepharoconjunctivitis), accompanied by small white itchy lesions on the surface of the cornea, which vary from minor damage to the epithelium (superficial punctate keratitis) to the formation of dendritic ulcers.[2] Infection is unilateral, affecting one eye at a time. Additional symptoms include dull pain deep inside the eye, mild to acute dryness, and sinusitis. Most primary infections resolve spontaneously in a few weeks or with the use of oral and topical antivirals. However, the virus continues to inhabit the neurons of the eye and to multiply.
Subsequent recurrences may be more severe, with infected epithelial cells showing larger dendritic ulceration and lesions forming white plaques.[2] The epithelial layer is sloughed off as the dendritic ulcer grows and mild inflammation (iritis) may occur in the underlying stroma of iris. Sensation loss occurs in lesional areas produces generalized corneal anaesthesia with repeated recurrences.[2] This may be accompanied by chronic dry eye, low-grade intermittent conjunctivitis, or chronic unexplained sinusitis. When the concentration of viral DNA reaches a critical limit, the presence of the virus can trigger a massive autoimmune response in the eye, resulting in an individual's immune system destroying the corneal stroma.[2] This usually results in loss of vision due to opacification of the cornea and is a result of an antibody response against the viral antigen expression in the stroma following persistent infection.[2] This is known as immune-mediated stromal keratitis.
Treatment
Surgery
Treatment with corneal transplants was once ineffective (with a 14-61% rate of survival without antiviral therapy), as reinfection of the transplant is common when the virus reactivates. However, with concurrent use of antivirals the chance of graft acceptance has improved.[3]
References
- ↑ Carr DJ, Härle P, Gebhardt BM (2001). "The immune response to ocular herpes simplex virus type 1 infection". Exp. Biol. Med. (Maywood). 226 (5): 353–66. PMID 11393165.
- ↑ 2.0 2.1 2.2 2.3 2.4 Suresh PS, Tullo AB (1999). "Herpes simplex keratitis". Indian J Ophthalmol. 47 (3): 155–65. PMID 10858770.
- ↑ Halberstadt M, Machens M, Gahlenbek KA, Böhnke M, Garweg JG (2002). "The outcome of corneal grafting in patients with stromal keratitis of herpetic and non-herpetic origin". Br J Ophthalmol. 86 (6): 646–52. PMID 12034687.