|
|
| (18 intermediate revisions by 2 users not shown) |
| Line 1: |
Line 1: |
| __NOTOC__ | | __NOTOC__ |
| | {{Infobox_Disease |
| | | Name = Autoimmune pancreatitis |
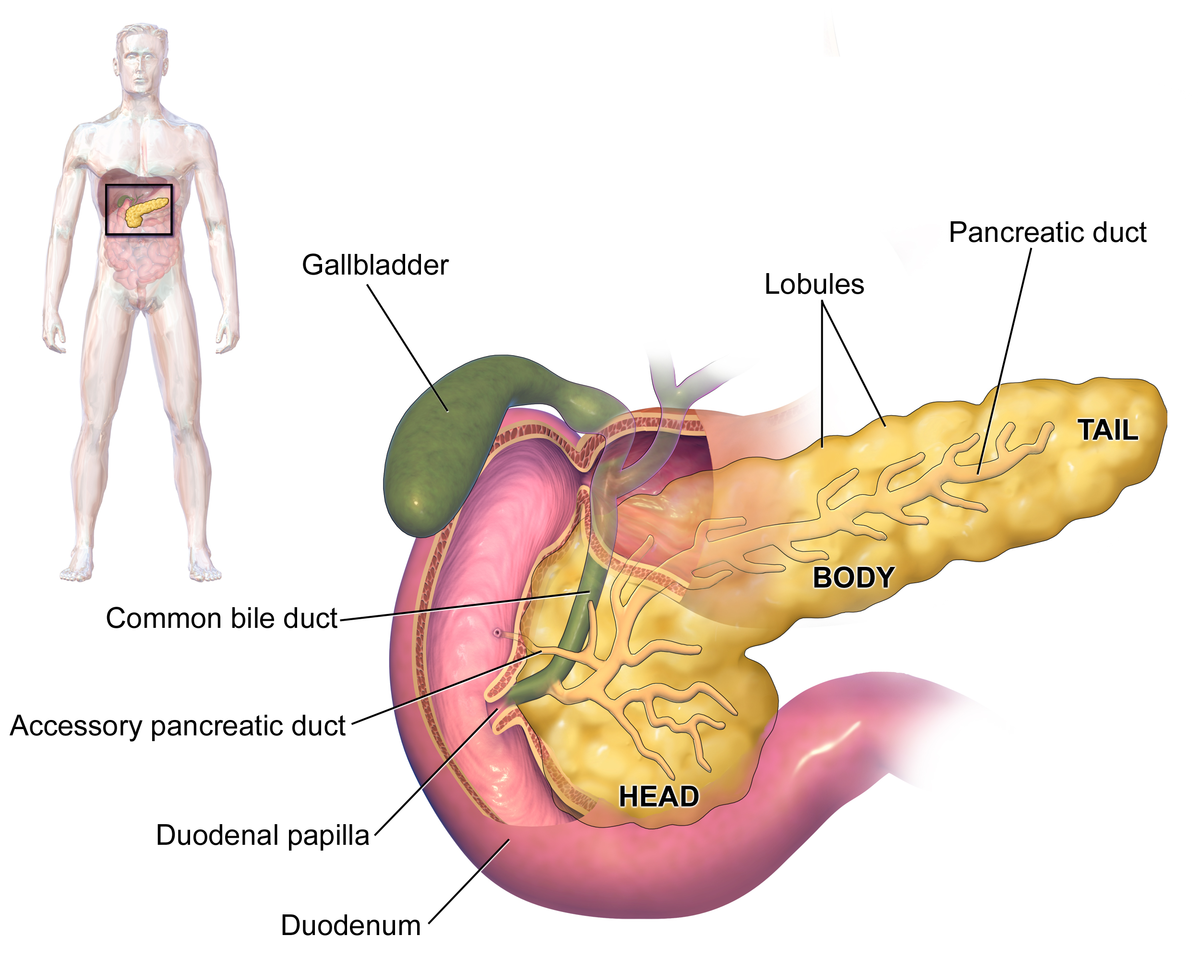
| | | Image = Blausen 0699 PancreasAnatomy2.png |
| | | Caption = Pancreas<ref><https://en.wikipedia.org/wiki/Pancreas#/media/File:Blausen_0699_PancreasAnatomy2.png></ref> |
| | }} |
| {{Autoimmune pancreatitis}} | | {{Autoimmune pancreatitis}} |
| {{CMG}}, {{AE}}:{{IQ}} | | {{CMG}}, {{AE}}:{{IQ}}{{FT}} |
|
| |
|
| ==Overview==
| | {{SK}} Primary inflammatory pancreatitis, Lymphoplasmacytic sclerosing pancreatitis, Pseudotumorous pancreatitis, Chronic pancreatitis with irregular narrowing of the main pancreatic duct, Nonalcoholic duct destructive chronic pancreatitis. |
| '''Autoimmune pancreatitis''' (AIP) is an increasingly recognized benign type of [[chronic pancreatitis]] that can be difficult to distinguish from [[pancreatic carcinoma]] but which responds to treatment with [[corticosteroids]].
| |
|
| |
|
| ==Historical Perspective== | | ==[[Autoimmune pancreatitis overview|Overview]]== |
|
| |
|
| ==Classification== | | ==[[Autoimmune pancreatitis historical perspective|Historical Perspective]]== |
|
| |
|
| ==Pathophysiology== | | ==[[Autoimmune pancreatitis classification|Classification]]== |
| Histopathologic examination of the pancreas reveals a characteristic lymphoplasmacytic infiltrate of [[CD4]]- or [[CD8]]-positive [[lymphocytes]] and IgG4-positive [[plasma cells]], and exhibits interstitial fibrosis and [[acinar cell]] atrophy in later stages. However, localization and the degree of duct wall infiltration are variable. Whereas histopathologic examination remains the primary method for differentiation of AIP from acute and chronic pancreatitis, [[lymphoma]], and cancer, little is known with regard to the cytopathologic diagnosis of AIP. It has been proposed that a cytologic smear rich in inflammatory cells ([[lymphocytes]], [[plasma cells]], [[granulocytes]]), with rare [[epithelial cells]] lacking atypia, favors the diagnosis of AIP. The sensitivity and the specificity of these criteria for differentiating AIP from neoplasia are unknown.
| |
|
| |
|
| ==Causes== | | ==[[Autoimmune pancreatitis pathophysiology|Pathophysiology]]== |
|
| |
|
| ==Differentiating Autoimmune Pancreatitis from other Diseases== | | ==[[Autoimmune pancreatitis causes|Causes]]== |
| As the number of published cases of AIP has increased, efforts have been focused on defining AIP as a distinct clinical and pathologic entity and toward developing some generally agreed upon diagnostic criteria and nomenclature. Terms frequently encountered are autoimmune or autoimmune-related pancreatitis, lymphoplasmacytic sclerosing pancreatitis, idiopathic tumefactive chronic pancreatitis, idiopathic pancreatitis with focal irregular narrowing of the main pancreatic duct, and non-alcoholic duct destructive chronic pancreatitis. There are also a large number of case reports employing descriptive terminology such as pancreatitis associated with [[Sjögren’s syndrome]], [[primary sclerosing cholangitis]], or [[inflammatory bowel disease]]. Some of the earliest cases were reported as pancreatic pseudotumor or [[pseudolymphoma]].
| |
|
| |
|
| ==Epidemiology and Demographics== | | ==[[Autoimmune pancreatitis differential diagnosis|Differentiating Sheehan's syndrome from other Diseases]]== |
|
| |
|
| ==Risk Factors== | | ==[[Autoimmune pancreatitis epidemiology and demographics|Epidemiology and Demographics]]== |
|
| |
|
| ==Natural History, Complications and Prognosis== | | ==[[Autoimmune pancreatitis risk factors|Risk Factors]]== |
|
| |
|
| ==Diagnosis== | | ==[[Autoimmune pancreatitis screening|Screening]]== |
| ===Diagnostic Criteria===
| |
| AIP is characterized by the following features: (1) mild symptoms ([[abdominal pain]], [[weight loss]], [[nausea]]), usually without acute attacks of [[pancreatitis]], (2) increased serum levels of gamma globulins, [[immunoglobulin G]] (IgG), or IgG4, (3) the presence of serum autoantibodies such as [[anti-nuclear antibody]] (ANA), anti-[[lactoferrin]] antibody, anti-[[carbonic anhydrase]] II antibody, and [[rheumatoid factor]] (RF), (4) a diffusely enlarged pancreas, (5) diffuse irregular narrowing of the main pancreatic duct and stenosis of the intrapancreatic bile duct on [[endoscopic retrograde cholangiopancreatography]] (ERCP), (6) rare pancreatic calcification or cyst formation, and (7) marked responsiveness to treatment with [[corticosteroids]]. AIP is sometimes associated with other autoimmune disorders, most commonly [[Sjögren's syndrome]], [[primary sclerosing cholangitis]] (PSC), and [[inflammatory bowel disease]]. AIP occurring in association with an [[autoimmune disorder]] has been referred to as “secondary” or “syndromic” AIP.
| |
|
| |
|
| In 2002, the Japanese Pancreas Society proposed the following diagnostic criteria for autoimmune pancreatitis:
| | ==[[Autoimmune pancreatitis natural history, complications and prognosis|Natural History, Complications and Prognosis]]== |
| ::I. Pancreatic imaging studies show diffuse narrowing of the main pancreatic duct with irregular wall (more than 1/3 of length of the entire pancreas).
| |
| ::II. Laboratory data demonstrate abnormally elevated levels of serum gamma globulin and/or [[IgG]], or the presence of [[autoantibodies]].
| |
| ::III. Histopathologic examination of the pancreas shows fibrotic changes with [[lymphocyte]] and [[plasma cell]] infiltrate.
| |
|
| |
|
| For diagnosis, criterion I (pancreatic imaging) must be present with criterion II (laboratory data) and/or III (histopathologic findings).
| | ==Diagnosis== |
| ===Symptoms=== | |
| ===Physical Examination===
| |
| ===Laboratory Findings===
| |
| ===Imaging Findings===
| |
| [[Computed tomography]] (CT) findings in AIP include a diffusely enlarged hypoechoic pancreas or a focal mass that may be mistaken for a pancreatic malignancy. A low-density, capsule-like rim on CT (possibly corresponding to an inflammatory process involving peripancreatic tissues) is thought to be an additional characteristic feature. [[Magnetic resonance imaging]] (MRI) reveals a diffusely decreased signal intensity and delayed enhancement on dynamic scanning. The characteristic [[ERCP]] finding is segmental or diffuse irregular narrowing of the main pancreatic duct, usually accompanied by an extrinsic-appearing stricture of the distal bile duct. Changes in the extrapancreatic bile duct similar to those of [[primary sclerosing cholangitis]] (PSC) have been reported.
| |
|
| |
|
| The role of [[endoscopic ultrasound]] (EUS) and EUS-guided [[fine-needle aspiration]] (EUS-FNA) in the diagnosis of AIP is not well described, and EUS findings have been described in only a small number of patients. In one study, EUS revealed a diffusely swollen and hypoechoic pancreas in 8 of the 14 (57%) patients, and a solitary, focal, irregular mass was observed in 6 (46%) patients. Whereas EUS-FNA is sensitive and specific for the diagnosis of pancreatic malignancy, its role in the diagnosis of AIP remains unclear.
| | [[Autoimmune pancreatitis diagnostic study of choice|Diagnostic Study of Choice]] | [[Autoimmune pancreatitis history and symptoms|History and Symptoms]] | [[Autoimmune pancreatitis physical examination|Physical Examination]] | [[Autoimmune pancreatitis laboratory findings|Laboratory Findings]] | [[Autoimmune pancreatitis x ray|X Ray]] | [[Autoimmune pancreatitis CT scan|CT]] | [[Autoimmune pancreatitis MRI|MRI]] | [[Autoimmune pancreatitis echocardiography and ultrasound|Echocardiography and Ultrasound]] | [[Autoimmune pancreatitis other imaging findings|Other Imaging Findings]] | [[Autoimmune pancreatitis other diagnostic studies|Other Diagnostic Studies]] |
| ===Other Diagnostic Studies===
| |
|
| |
|
| ==Treatment== | | ==Treatment== |
| ===Medical Therapy===
| | |
| AIP often completely resolves with steroid treatment. The failure to differentiate AIP from malignancy may lead to unnecessary pancreatic resection, and the characteristic lymphoplasmacytic infiltrate of AIP has been found in up to 23% of patients undergoing pancreatic resection for suspected malignancy who are ultimately found to have benign disease. In this subset of patients, a trial of steroid therapy may have prevented a [[Whipple procedure]] or complete [[pancreatectomy]] for a benign disease which responds well to medical therapy.
| | [[Autoimmune pancreatitis medical therapy|Medical Therapy]] | [[Autoimmune pancreatitis surgery|Surgery]] | [[Autoimmune pancreatitis primary prevention|Primary Prevention]] | [[Autoimmune pancreatitis secondary prevention|Secondary Prevention]] | |
| ===Surgery===
| |
| ===Prevention===
| |
|
| |
|
| ==References== | | ==References== |