Adult bronchiolitis pathophysiology
|
Adult bronchiolitis Microchapters |
|
Differentiating Occupational lung disease from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Adult bronchiolitis pathophysiology On the Web |
|
American Roentgen Ray Society Images of Adult bronchiolitis pathophysiology |
|
|
|
Risk calculators and risk factors for Adult bronchiolitis pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Hadeel Maksoud M.D.[2]
Overview
The pathogenesis of adult bronchiolitis is to be the result of inflammation and immunological responses that cause cellular injury and damage. Eventually, respiratory compromise results, which may be irreversible and fatal. Associated conditions include asthma and primary immunodeficiencies. The gross pathology of bronchiolitis includes bronchiolar and airway destruction. Microscopically, fibroblasts and lymphocytes are noted.
Pathophysiology
Pathogenesis
- The bronchioles are the terminal conducting airways that lack in cartilage and glands.[1][2][3]
- The bronchioles are of 2mm in diameter.
- The area of gas exchange known as the acinus is made up of three parts, the respiratory bronchiole, the alveolar duct and the alveolus.
- The respiratory bronchiole contains Clara cells and neuroendocrine cells, which produce somatostatin and serotonin.
- When an assault towards the bronchioles happens whether infectious or irritant in origin, an inflammatory process will begin followed by an immunological response which results in bronchiolitis.
- Immediately following exposure cellular destruction begins with the release of proteolytic enzymes and IgE in a type I hypersensitivity reaction.
- The initial inflammatory reaction leads to:
- Increased mucus secretion
- Due to goblet proliferation
- Bronchial constriction
- Alveolar cell death
- Mucosal debris
- Increased airway resistance
- Increased mucus secretion
- Within 18 - 24 hours the effects of an irritant or infection begin to appear.
- The infected epithelial cells lining the bronchioles begin to release chemokines and cytokines, this augments the immune response leads to the production of interferon and interleukins 4, 8 and 9.
- The immune response leads to:
- Bronchial obstruction
- Ventilation-perfusion mismatch
- Dyspnea
- Necrosis of respiratory epithelium
- Atelectasis
- Due to destruction of cilia
- Lymphocytic filtration
- Leads to submucosal edema
- Hyperinflation
- Repair is eventually started with the establishment of granulation tissue in place of the damage cells
- May result in permanent fibrosis, which may be submucosal or peribronchiolar and therefore, obliterates the bronchiolar lumen.
- May also result in complete resolution
Genetics
- Genetic susceptibility is thought to play a large role in the pathogenesis of infantile bronchiolitis and will not be discussed here.
- However, age-related genetics may be implicated in the development of bronchiolitis in the elderly.
Associated Conditions
- Asthma
- Primary immunodeficiencies
- Such as severe combined immunodeficiency
- Immunodeficient states
- Such as elderly and smokers
- Congenital bronchopulmonary dysplasia
- Pre-exisiting cardiovascular or pulmonary lung disease
- Rheumatoid arthritis
- Heart/lung/kidney transplant
Gross Pathology
- On gross pathology, (thickened bronchial walls) increased reticular markings, fibrous tissue proliferation, and airway destruction are characteristic findings of adult bronchiolitis.
Microscopic Pathology
- On microscopic histopathological analysis, fibroblasts, macrophages, and lymphocytes and plasma cells are characteristic findings of adult bronchiolitis.
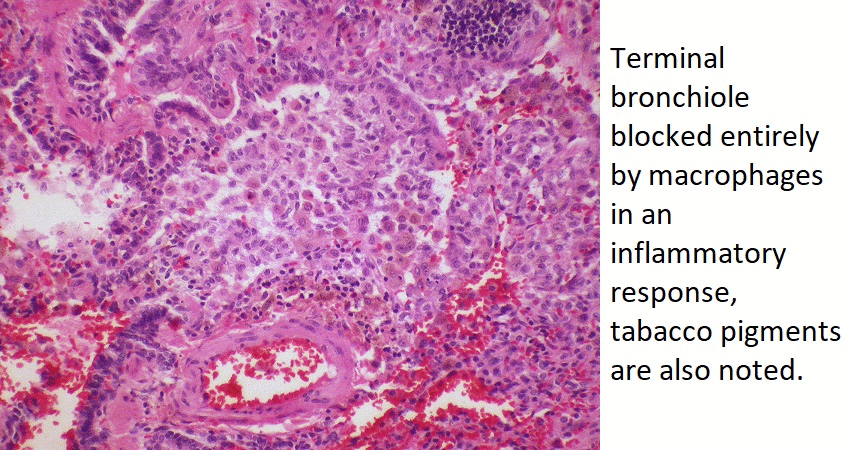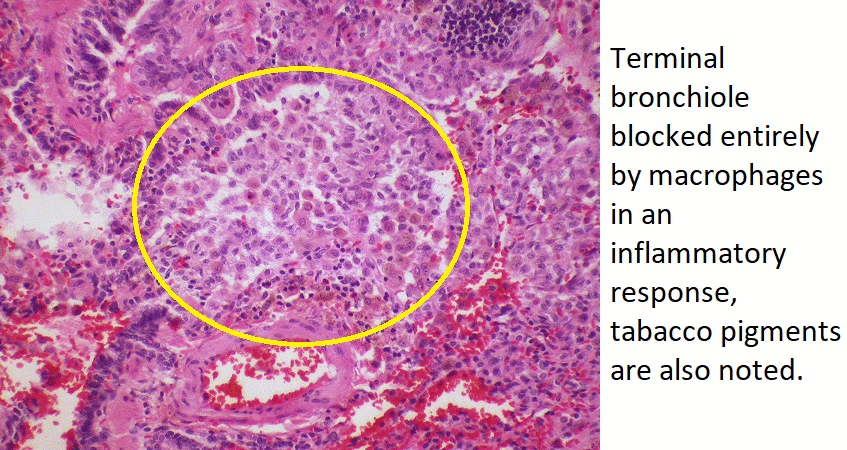
References
- ↑ McNamara PS, Flanagan BF, Hart CA, Smyth RL (April 2005). "Production of chemokines in the lungs of infants with severe respiratory syncytial virus bronchiolitis". J. Infect. Dis. 191 (8): 1225–32. doi:10.1086/428855. PMID 15776367.
- ↑ Visscher DW, Myers JL (2006). "Bronchiolitis: the pathologist's perspective". Proc Am Thorac Soc. 3 (1): 41–7. doi:10.1513/pats.200512-124JH. PMID 16493150.
- ↑ Couture C, Colby TV (October 2003). "Histopathology of bronchiolar disorders". Semin Respir Crit Care Med. 24 (5): 489–98. doi:10.1055/s-2004-815600. PMID 16088569.