Endometrium
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
The endometrium is the inner membrane of the mammalian uterus.
Function
The endometrium functions as a lining for the uterus, preventing adhesions between the opposed walls of the myometrium, thereby maintaining the patency of the uterine cavity. During the menstrual cycle or estrous cycle, the endometrium grows to a thick, blood vessel rich, glandular tissue layer. This represents an optimal environment for the implantation of a blastocyst upon its arrival in the uterus.
During pregnancy, the glands and blood vessels in the endometrium further increase in size and number. Vascular spaces fuse and become interconnected, forming the placenta, which supplies oxygen and nutrition to the embryo and fetus.
Cycle
The endometrial lining undergoes cyclic regeneration. Humans and the great apes display the menstrual cycle, whereas most other mammals are subject to an estrous cycle. In both cases, the endometrium initially proliferates under the influence of estrogen. However, once ovulation occurs, in addition to estrogen, the ovary will also start to produce progesterone. This changes the proliferative pattern of the endometrium to a secretory lining. Eventually, the secretory lining provides a hospitable environment for one or more blastocysts.
If no blastocyst is detected, the progesterone level drops and the endometrial lining is either reabsorbed (estrous cycle) or shed (menstrual cycle). In the latter case, the process of shedding involves the breaking down of the lining, the tearing of small connective blood vessels, and the loss of the tissue and blood that had constituted it through the vagina. The entire process occurs over a period of several days. Menstruation may be accompanied by a series of uterine contractions; these help expel the menstrual endometrium.
In case of implantation, however, the endometrial lining is neither absorbed nor shed. Instead, it remains as decidua. The decidua becomes part of the placenta; it provides support and protection for the gestation.
If there is inadequate stimulation of the lining, due to lack of hormones, the endometrium remains thin and inactive. In humans, this will result in amenorrhea. After menopause, the lining is often described as being atrophic. In contrast, endometrium that is chronically exposed to estrogens, but not to progesterone, may become hyperplastic.
In humans, the cycle of building and shedding the endometrial lining lasts an average of 28 days. The endometrium develops at different rates in different mammals. Its formation is sometimes affected by seasons, climate, stress and other factors. The endometrium itself produces certain hormones at different points along the cycle. This affects other portions of the reproductive system.
Histology
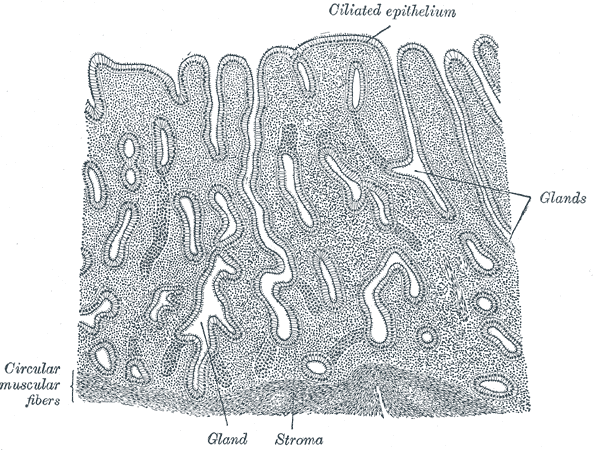
The endometrium consists of a single layer of columnar epithelium, resting on a layer of connective tissue which varies in thickness according to hormonal influences - the stroma. Simple tubular uterine glands reach from the endometrial surface through to the base of the stroma, which also carries a rich blood supply of spiral arteries. In a woman of reproductive age, two layers of endometrium can be distinguished. These two layers occur only in endometrium lining the cavity of the uterus, not in the lining of the Fallopian tubes:[1]
- The functional layer is adjacent to the uterine cavity. This layer is built up after the end of menstruation during the first part of the previous menstrual cycle. Proliferation is induced by progesterone (follicular phase of menstrual cycle), and later increased by the progestrone from the corpus luteum (luteal phase). It is adapted to provide an optimum environment for the implantation and growth of the embryo. This layer is completely shed during menstruation.
- The basal layer, adjacent to the myometrium and below the functional layer, is not shed at any time during the menstrual cycle, and from it the functional layer develops.
In the absence of progesterone, the arteries supplying blood to the functional layer constrict, so that cells in that layer become ischaemic and die, leading to menstruation.
It is possible to identify the phase of the menstrual cycle by observing histological differences at each phase:
| Phase | Days | Thickness | Epithelium |
| menstrual phase | 1-4 | thin | absent |
| proliferative phase | 4-14 | intermediate | columnar |
| secretory phase | 15-28 | thick | columnar. Also visible are helicine branches of uterine artery |
Pathological conditions
Adenomyosis is the growth of the endometrium into the muscle layer of the uterus (the myometrium).
Endometriosis is the growth of endometrial tissue outside the uterus.
Endometrial cancer is the most common cancer of the human female genital tract.
See also
Additional images
-
Vertical section of mucous membrane of human uterus.
-
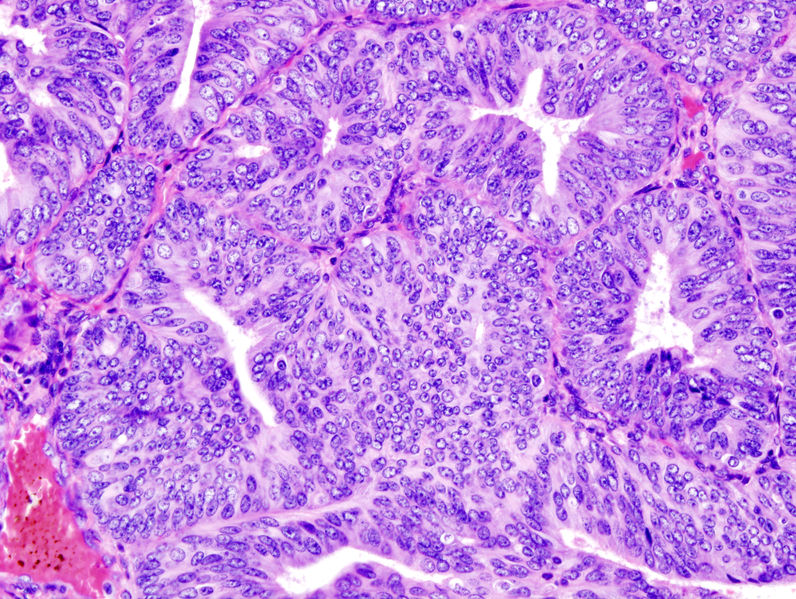
Histopathologic representation of endometrioid adenocarcinoma demonstrated in endometrial biopsy. Hematoxylin-eosin stain.
-
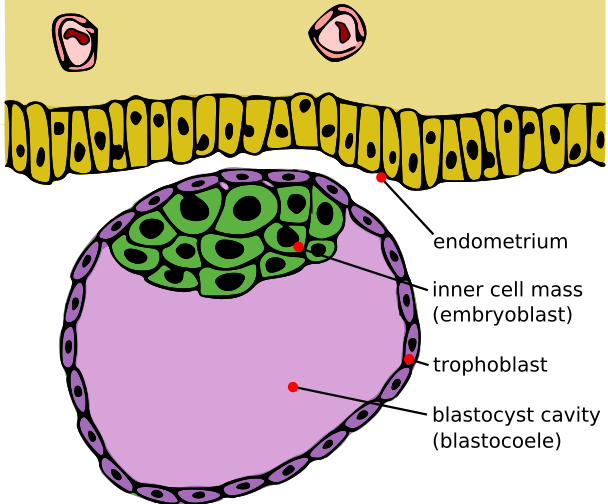
Blastocyst with an inner cell mass and trophoblast.
-
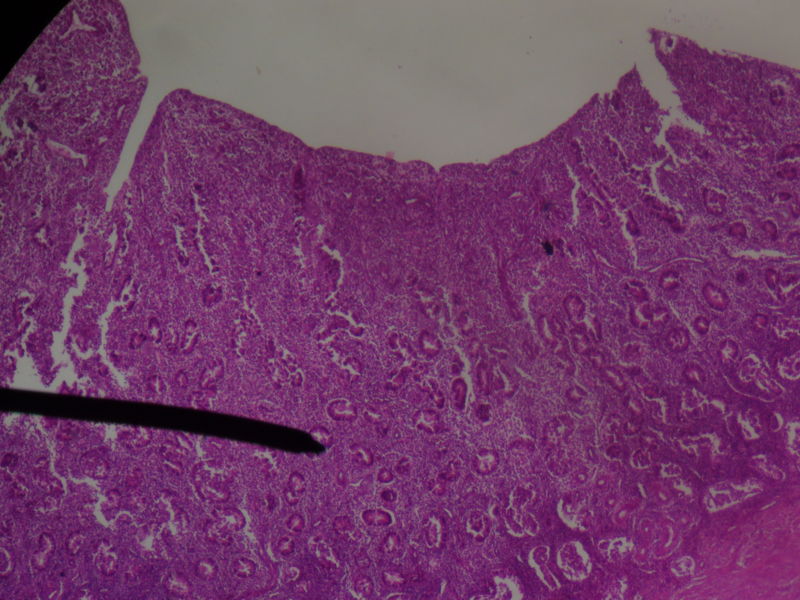
microscopic slide of the endometrium.
References
- ↑ Blue Histology - Female Reproductive System. School of Anatomy and Human Biology - The University of Western Australia http://www.lab.anhb.uwa.edu.au/mb140/CorePages/FemaleRepro/FemaleRepro.htm Accessed 20061228 20:35
External links
- Template:SUNYAnatomyFigs - "The uterus, uterine tubes and ovary with associated structures."
- Histology image: 18902loa – Histology Learning System at Boston University - "Female Reproductive System uterus, endometrium"
- Template:EmbryologySwiss
- Template:OklahomaHistology
- Histology at utah.edu. Slide is proliferative phase - click forward to see secretory phase
Template:Female reproductive system
ar:بطانة الرحم de:Endometrium it:Endometrio lt:Endometriumas nl:Endometrium no:Endometrium simple:Endometrium sv:Livmoderslemhinna