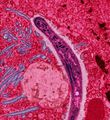
Plasmodium
|
Malaria Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case studies |
|
Plasmodium On the Web |
|
American Roentgen Ray Society Images of Plasmodium |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
- A plasmodium is also the macroscopic form of the protist known as a slime mould.
Plasmodium is a genus of parasitic protozoa. Infection with this genus is known as malaria. The parasite always has two hosts in its life cycle: a mosquito vector and a vertebrate host. At least ten species infect humans. Other species infect other animals, including birds, reptiles and rodents.
Taxonomy and host range
The genus Plasmodium was created in 1885 by Marchiafava and Celli and there are over 175 species currently recognized. New species continue to be described. [1]
The genus is currently (2006) in need of reorganization as it has been shown that parasites belonging to the genera Haemocystis and Hepatocystis appear to be closely related to Plasmodium. It is likely that other species such as Haemoproteus meleagridis will be included in this genus once it is revised.
Host range among the mammalian orders is non uniform. At least 29 species infect non human primates; rodents outside the tropical parts of Africa are rarely affected; a few species are known to infect bats, porcupines and squirrels; carnivores, insectivores and marsupials are not known to act as hosts.
In 1898 Ronald Ross demonstrated the existence of Plasmodium in the wall of the midgut and salivary glands of a Culex mosquito. For this discovery he won the Nobel Prize in 1902. However credit must also be given to the Italian professor Giovanni Battista Grassi, who showed that human malaria could only be transmitted by Anopheles mosquitoes. It is worth noting, however, that for some species the vector may not be a mosquito.
Mosquitoes of the genera Culex, Anopheles, Culiceta, Mansonia and Aedes may act as vectors. The currently known vectors for human malaria (> 100 species) all belong to the genus Anopheles. Bird malaria is commonly carried by species belonging to the genus Culex. Only female mosquitoes bite. Aside from blood both sexes live on nectar, but one or more blood meals are needed by the female for egg laying as the protein content of nectar is very low. The life cycle of Plasmodium was discovered by Ross who worked with species from the genus Culex.
The life cycle of Plasmodium is very complex. Sporozoites from the saliva of a biting female mosquito are transmitted to either the blood or the lymphatic system[2] of the recipient. The sporozoites then migrate to the liver and invade hepatocytes. This latent or dormant stage of the Plasmodium sporozoite in the liver is called the hypnozoite.
The development from the hepatic stages to the erythrocytic stages has until very recently been obscure. In 2006[3] it was shown that the parasite buds off the hepatocytes in merosomes containing hundreds or thousands of merozoites. These merosomes have been subsequently shown[4] to lodge in the pulmonary capilaries and to slowly disintergrate there over 48-72 hours releasing merozoites. Erythrocyte invasion is enhanced when blood flow is slow and the cells are tightly packed: both of these conditions are found in the alveolar capilaries.
Within the erythrocytes the merozoite grow first to a ring-shaped form and then to a larger trophozoite form. In the schizont stage, the parasite divides several times to produce new merozoites, which leave the red blood cells and travel within the bloodstream to invade new red blood cells. Most merozoites continue this replicative cycle, but some merozoites differentiate into male or female sexual forms (gametocytes) (also in the blood), which are taken up by the female mosquito.
In the mosquito's midgut, the gametocytes develop into gametes and fertilize each other, forming motile zygotes called ookinetes. The ookinetes penetrate and escape the midgut, then embed themselves onto the exterior of the gut membrane. Here they divide many times to produce large numbers of tiny elongated sporozoites. These sporozoites migrate to the salivary glands of the mosquito where they are injected into the blood of the next host the mosquito bites. The sporozoites move to the liver where they repeat the cycle.
Reactivation of the hypnozoites has been reported for up to 30 years after the initial infection in humans. The factors precipating this reactivation are not known. In the species Plasmodium malariae, Plasmodium ovale and Plasmodium vivax hypnozoites have been shown to occur. Reactivation does not occur in infections with Plasmodium falciparum. It is not known if hypnozoite reactivaction may occur with any of the remaining species that infect humans but this is presumed to be the case.
Evolution
This life cycle is best understood in terms of its evolution.
The Apicomplexia - the phylum to which Plasmodium belongs - are thought to have originated within the Dinoflagellates - a large group of photosynthetic protozoa. It is currently thought that the ancestors of the Apicomplexia were originally prey organisms that evolved the ability to invade the intestinal cells and subsequently lost their photosynthetic ability. Some extant dinoflagelates, however, can invade the bodies of jellyfish and continue to photosynthesize, which is possible because jellyfish bodies are almost transparent. In other organisms with opaque bodies this ability would most likely rapidly be lost.
It is thought that Plasmodium evolved from a parasite spread by the orofaecal route which infected the intestinal wall. At some point this parasite evolved the ability to infect the liver. This pattern is seen in the genus Cryptosporidium to which Plasmodium is distantly related. At some later point this ancestor developed the ability to infect blood cells and to survive and infect mosquitoes. Once mosquito transmission was firmly established the previous orofecal route of transmission was lost.
Current (2007) theory suggests that the genera Plasmodium, Hepatocystis and Haemoproteus evolved from Leukocytozoon species. Parasites of the genus Leukocytozoan infect white blood cells (leukocytes), liver and spleen cells and are transmitted by 'black flies' (Simulium species) - a large genus of flies related to the mosquitoes.
Leukocytes, hepatocytes and most spleen cells actively phagocytose particulate matter making entry into the cell easier for the parasite. The mechanism of entry of Plasmodium species into erythrocytes is still very unclear taking as it does less than 30 seconds. It is not yet known if this mechanism evolved before mosquitoes became the main vectors for transmission of Plasmodium.
Plasmodium evolved about 130 million years ago. This period is coincidental with the rapid spread of the angiosperms (flowering plants). This expansion in the angiosperms is thought to be due to at least one genomic duplication event. It seems probable that the increase in the number of flowers led to an increase in the number of mosquitoes and their contact with vertebrates.
Mosquitoes evolved in what is now South America about 230 million years ago. There are over 3500 species recognised but to date their evolution has not been well worked out so a number of gaps in our knowledge of the evolution of Plasmodium remain.
Presently it seems probable that birds were the first group infected by Plasmodium followed by the reptiles - probably the lizards. At some point primates and rodents became infected. The remaining species infected outside these groups seem likely to be due to relatively recent events.
At the present time (2007) DNA sequences are available from fewer than sixty species and most of these are from species infecting either rodent or primate hosts. The evolution proposed here should be regarded as speculative and subject to revision as data becomes available.
Reproduction
The pattern of alternation of sexual and asexual reproduction which may seem confusing at first is a very common pattern in parasitic species. The evolutionary advantages of this type of life cycle were recognised by Mendel.
Under favourable conditions asexual reproduction is superior to sexual as the parent is well adapted to its environment and its descendents share these genes. Transferring to a new host or in times of stress, sexual reproduction is generally superior as this produces a shuffling of genes which on average at a population level will produce individuals better adapted to the new environment.
Molecular biology
All the species examined to date have 14 chromosomes, one mitochondrion and one plastid. The chromosomes vary from 500 kilobases to 3.5 megabases in length. It is presumed that this is the pattern throughout the genus.
The plastid unlike those found in algae is not photosynthetic. Its function is not known but there is some suggestive evidence that it may be involved in reproduction.
On a molecular level, the parasite damages red blood cells using plasmepsin enzymes - aspartic acid proteases which degrade hemoglobin.
Diagnostic characteristics of the genus Plasmodium
- Forms gamonts in erythrocytes
- Merogony occurs in erythrocytes and in other tissues
- Hemozoin is present
- Vectors are either mosquitos or sandflies
- Vertebrate hosts include mammals, birds and reptiles
Taxonomy
Plasmodium belongs to the family Plasmodiidae (Levine, 1988), order Haemosporidia and phylum Apicomplexia. There are currently 450 recognised species in this order. Many species of this order are undergoing reexamination of their taxonomy with DNA analysis. It seems likely that many of these species will be re assigned after these studies have been completed.[5][6] For this reason the entire order is outlined here.
Notes:
The genera Plasmodium, Fallisia and Saurocytozoon all cause malaria in lizards. All are carried by Dipteria (roughly speaking the flies). Pigment is absent in the Garnia. Non pigmented gametocytes are typically the only forms found in Saurocytozoon: pigmented forms may be found in the leukocytes occasionally. Fallisia produce non pigmented asexual and gametocyte forms in leukocytes and thrombocytes.
Subgenera
The full taxonomic name of a species includes the subgenus but this is often omitted. The full name indicates some features of the morphology and type of host species.
The only two species in the sub genus Laverania are P. falciparum and P. reichenowi.
Species infecting monkeys and apes (the higher primates) with the exceptions of P. falciparum and P. reichenowi are classified in the subgenus Plasmodium.
Parasites infecting other mammals including lower primates (lemurs and others) are classified in the subgenus Vinckeia.
The distinction between P. falciparum and P. reichenowi and the other species infecting higher primates was based on the morphological findings but have since been confirmed by DNA analysis. Vinckeia while previously considered to be something of a taxonomic 'rag bag' has been recently shown - perhaps rather surprisingly - to form a coherent grouping.
The remaining groupings here are based on the morphology of the parasites. Revisions to this system are likely to occur in the future as more species are subject to analysis of their DNA.
The four subgenera Giovannolaia, Haemamoeba, Huffia and Novyella were created by Corradetti et al[7] for the known avian malarial species. A fifth - Bennettinia - was created in 1997 by Valkiunas.[8] The relationships between the subgenera are the matter of current investigation. Martinsen et al 's recent (2006) paper outlines what is currently (2007) known.[9]
P. juxtanucleare is currently (2007) the only known member of the subgenus Bennettinia.
Unlike the mammalian and bird malarias those affecting reptiles have been more difficult to classify. In 1966 Garnham classified those with large schizonts as Sauramoeba, those with small schizonts as Carinamoeba and the single then known species infecting snakes (Plasmodium wenyoni) as Ophidiella.[10] He was aware of the arbitrariness of this system and that it might not prove to be biologically valid. Telford in 1988 used this scheme as the basis for the currently accepted (2007) system.[11]
Classification criteria
Species in the subgenus Bennettinia have the following characteristics:
- Schizonts contain scant cytoplasm, are often round, do not exceed the size of the host nucleus and stick to it.
- Gametocytes while varying in shape tend to be round or oval, do not exceed the size of the nucleus and stick to it.
Species in the subgenus Giovanolaia have the following characteristics:
- Schizonts contain plentiful cytoplasm, are larger than the host cell nucleus and frequently displace it. They are found only in mature erythrocytes.
- Gametocytes are elongated.
- Exoerythrocytic schizogony occurs in the mononuclear phagocyte system.
Species in the subgenus Haemamoeba have the following characteristics:
- Mature schizonts are larger than the host cell nucleus and commonly displace it.
- Gametocytes are large, round, oval or irregular in shape and are substantially larger than the host nucleus.
Species in the subgenus Huffia have the following characteristics:
- Mature schizonts, while varying in shape and size, contain plentiful cytoplasm and are commonly found in immature erthryocytes.
- Gametocytes are elongated.
Species in the subgenus Novyella have the following characteristics:
- Mature schisonts are either smaller than or only slightly larger than the host nucleus. They contain scanty cytoplasm.
- Gametocytes are elongated. Sexual stages in this subgenus resemble those of Haemoproteus.
- Exoerythrocytic schizogony occurs in the mononuclear phagocyte system
Species in the subgenus Carinamoeba have the following characteristics:
- Infect lizards
- Schizonts normally give rise to less than 8 merozoites
Species in the subgenus Sauramoeba have the following characteristics:
- Infect lizards
- Schizonts normally give rise to more than 8 merozoites
Notes
- The erythrocytes of both reptiles and birds retain their nucleus, unlike those of mammals. The reason for the loss of the nucleus in mammalian erythocytes remains unknown.
- The presence of elongated gametocytes in several of the avian subgenera and in Laverania in addition to a number of clinical features suggested that these might be closely related. This is is no longer thought to be the case.
- Plasmodium falciparum (the cause of malignant tertian malaria)
- Plasmodium vivax (the most frequent cause of benign tertian malaria)
- Plasmodium ovale (the other, less frequent, cause of benign tertian malaria)
- Plasmodium malariae (the cause of benign quartan malaria)
- Plasmodium knowlesi
- Plasmodium brasilianum
- Plasmodium cynomolgi
- Plasmodium cynomolgi bastianellii
- Plasmodium inui
- Plasmodium rhodiani
- Plasmodium schweitzi
- Plasmodium semiovale
- Plasmodium simium
The first four listed here are the most common species that infect humans. With the use of the polymerase chain reaction additional species have been and are still being identified that infect humans.
One possible experimental infection has been reported with Plasmodium eylesi. Fever and low grade parasitemia were apparent at 15 days. The volunteer (Dr Bennett) had previously been infected by Plasmodium cynomolgi and the infection was not transferable to a gibbon (P. eylesi 's natural host) so this cannot be regarded as definitive evidence of its ability to infect humans. A second case has been reported that may have been a case of P. eylesi but the author was not certain of the infecting species.[12]
A possible infection with Plasmodium tenue has been reported. [13] This report described a case of malaria in a three year old black girl from Georgia, USA who had never been outside the US. She suffered from both P. falciparum and P. vivax malaria and while forms similar to those described for P. tenue were found in her blood even the author was skeptical about the validity of the diagnosis. Confusingly Plasmodium tenue was proposed in the same year (1914) for a species found in birds. The human species is now considered to be likely to have been a misdiagnosis and the bird species is described on the Plasmodium tenue page.
Notes:
The only known host of P. falciparum are humans; neither is any other host currently known for P. malariae.
P. vivax will infect chimpanzees. Infection tends to be low grade but may be persistent and remain as source of parasites for humans for some time. P. vivax is also known to infect orangutans.[14]
Like P. vivax, P. ovale has been shown to be transmittable to chimpanzees. P. ovale has a unusual distribution pattern being found in Africa, the Philippines and New Guinea. In spite of its admittedly poor transmission to chimpanzees given its discontigous spread, it is suspected that P. ovale may in fact be a zooenosis with an as yet unidentified host. If this is actually the case, the host seems likely to be a primate.
The remaining species capable of infecting humans all have other primate hosts.
Plasmodium shortii and Plasmodium osmaniae are now considered to be junior synonyms of Plasmodium inui
Species no longer recognised as valid
Taxonomy in parasitology until the advent of DNA based methods has always been a problem and revisions in this area are continuing. A number of synonoms have been given for the species infecting humans that are no longer recognised as valid.[15] Since perusal of the older literature may be confusing some of these are listed here...
The species that infect primates other than humans include: P. bouillize, P. brasilianum, P. bucki, P. cercopitheci,P. coatneyi, P. coulangesi, P. cynomolgi, P. eylesi, P. fieldi, P. foleyi, P. fragile, P. girardi, P. georgesi, P. gonderi, P. hylobati, P. inui, P. jefferyi, P. joyeuxi,P. knowlesi, P. lemuris, P. percygarnhami, P. petersi, P. reichenowi, P. rodhaini, P. sandoshami, P. semnopitheci, P. silvaticum, P. simiovale, P. simium, P. uilenbergi, P. vivax and P. youngei.
Host records - Most if not all Plasmodium species infect more than one host: the host records shown here should be regarded as being incomplete.
References
- ↑ Chavatte JM, Chiron F, Chabaud A, Landau I. (2007) Probable speciations by "host-vector 'fidelisation'": 14 species of Plasmodium from Magpies. Parasite 14(1):21-37
- ↑ [http://www.hhmi.org/news/menard20060122.html HHMI Staff (22 January 2006) "Malaria Parasites Develop in Lymph Nodes" HHMI News Howard Hughes Medical Institute
- ↑ Sturm A, Amino R, van de Sand C, Regen T, Retzlaff S, Rennenberg A, Krueger A, Pollok JM, Menard R, Heussler VT. (2006) Manipulation of host hepatocytes by the malaria parasite for delivery into liver sinusoids. Science 313(5791):1287-1290
- ↑ Baer K, Klotz C, Kappe SH, Schnieder T, Frevert U. (2007) Release of Hepatic Plasmodium yoelii Merozoites into the Pulmonary Microvasculature. PLoS Pathog. 3(11):e171
- ↑ Perkins SL, Schall JJ (2002) A molecular phylogeny of malarial parasites recovered from cytochrome b gene sequences. J. Parasitology 88 (5): 972-978
- ↑ Yotoko, K. S. C. and Elisei C. (2006) Malaria parasites (Apicomplexa, Haematozoea) and their relationships with their hosts: is there an evolutionary cost for the specialization? J. Zoo. Syst. Evol. Res. 44 (4) 265
- ↑ Corradetti A., Garnham P. C. C. and Laird M. (1963). New classification of the avian malaria parasites. Parassitologia 5, 1–4
- ↑ Valkiunas, G. (1997). Bird Haemosporidia. Institute of Ecology, Vilnius
- ↑ Martinsen,E. S., Waite J. L. and Schall J. J. (2006) Morphologically defined subgenera of Plasmodium from avian hosts: test of monophyly by phylogenetic analysis of two mitochondrial genes. Parasitology 1-8
- ↑ Garnham P.C.C. (1966) Malaria parasites and other haemospordia. Oxford, Blackwell
- ↑ Telford S. (1988) A contribution to the systematics of the reptilian malaria parasites, family Plasmodiidae (Apicomplexa: Haemosporina). Bulletin of the Florida State Museum Biological Sciences 34, 65-96
- ↑ Tsukamoto M. (1977) An imported human malarial case characterized by severe multiple infections of the red blood cells. Ann. Trop. Med. Parasit. 19(2)95-104
- ↑ Russel P.F. (1928) Plasmodium tenue (Stephens): A review of the literature and a case report. Am. J. Trop. Med. s1-8(5) 449-479
- ↑ Reid MJ. (2006) Transmission of Human and Macaque Plasmodium spp. to Ex-Captive Orangutans in Kalimantan, Indonesia. Emerg Infect Dis. 12(12):1902-1908
- ↑ Coatney G. R. and Roudabush R. L. (1936) A catalog and host-index of the genus Plasmodium. J. Parasitol. 22 (4) 338-353
Template:SIB ar:متصورة ca:Plasmodi de:Plasmodium eo:Plasmodio hr:Plasmodium id:Plasmodium it:Plasmodium he:Plasmodium lt:Plazmodis ms:Plasmodium sr:Plasmodium sv:Plasmodium (släkte) ta:பிளாஸ்மோடியம் th:พลาสโมเดียม