Diabetes mellitus type 1 laboratory findings
|
Diabetes mellitus type 1 Microchapters |
|
Differentiating Diabetes mellitus type 1 from other Diseases |
|
Diagnosis |
|
Treatment |
|
Cardiovascular Disease and Risk Management |
|
Case Studies |
|
Diabetes mellitus Main page |
|
Patient Information |
|---|
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Vishal Devarkonda, M.B.B.S[2]
Overview
Laboratory findings consistent with the diagnosis of type 1 DM include FPG ≥126 mg/dL (7.0 mmol/L), or 2-h PG ≥200 mg/dL (11.1 mmol/L) during an OGTT, or A1C ≥6.5% (48 mmol/mol), or classic symptoms of hyperglycemia or hyperglycemic crisis, a random plasma glucose ≥200 mg/dL (11.1 mmol/L).
Laboratory Findings
Laboratory findings consistent with the diagnosis of type 1 DM include:[1][2][3]
| ADA Criteria for the diagnosis of diabetes |
|---|
| FPG ≥126 mg/dL (7.0 mmol/L). Fasting is defined as no caloric intake for at least 8 h.* |
| OR |
| 2-h PG ≥200 mg/dL (11.1 mmol/L) during an OGTT. The test should be performed as described by the WHO, using a glucose load containing the equivalent of 75 g anhydrous glucose dissolved in water.* |
| OR |
| A1C ≥6.5% (48 mmol/mol). The test should be performed in a laboratory using a method that is NGSP certified and standardized to the DCCT assay.* |
| OR |
| In a patient with classic symptoms of hyperglycemia or hyperglycemic crisis, a random plasma glucose ≥200 mg/dL (11.1 mmol/L). |
↵* In the absence of unequivocal hyperglycemia, results should be confirmed by repeat testing.
| Laboratory findings in type 1 diabetes based on presentation | |||
|---|---|---|---|
| Classic new onset | Diabetic Ketoacidosis | ||
| Blood | Glucose |
|
Random glucose level is more then 250 mg/dl |
| HbA1C | HbA1c level of 6.5% or higher | Not applicable | |
| C-Peptide below | below 5 µU/mL | Not applicable | |
| Islet-cell (IA2) | Measurements of IA2 autoantibodies within 6 months of diagnosis can help differentiate between type 1 and type 2 DM | Not applicable | |
| Anti-GAD65 | Usually present | Not applicable | |
| Anti-insulin autoantibodies | Usually present | Not applicable | |
| CBC with differential | Normal | Mildly elevated with normal differential | |
| Basic metabolic panel | Normal | Serum bicarbonate < 18 mEq/L
Serum Sodium: Often normal or elevated Serum Phosphate: Often normal or elevated Serum Potassium: Often normal or elevated | |
| Serum Creatinine | Normal | Often elevated | |
| Serum calicum | Normal | Decreased | |
| Serum amylase | Normal | Mildly elevated | |
| Serum Lipase | Normal | Normal | |
| Serum osmorality | Normal | Normal | |
| Serum Ketones | Normal | High | |
| Anion gap | normal | High | |
| Arterial Blood gas | Normal | Metabolic acidosis, compensated by | |
| Urine | Glucose | May or may not be present, (blood glucose should be more then 200 mg/dl to appear in urine) | Often present |
| Ketones | absent | Present | |
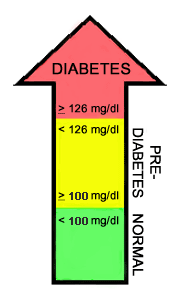
FPG OGTT
- IA2, GAD65 and insulin autoantibodies have been detected numerous months or years before the type 1 diabetes mellitus onset. This fact leads to the idea of using these autoantibodies as predictive tools for individuals at risk of developing clinical disease. Chance of developing type 1 diabetes mellitus within 5 years was ∼10%, ∼50% and 60–80% in the presence of one, two or three autoantibodies respectively, based on one study.[4]
References
- ↑ Type 1 Diabetes mellitus "Dennis Kasper, Anthony Fauci, Stephen Hauser, Dan Longo, J. Larry Jameson, Joseph Loscalzo"Harrison's Principles of Internal Medicine, 19e Accessed on December 27th,2016
- ↑ "NIDDK".
- ↑ Karaguzel G, Ozer S, Akcurin S, Turkkahraman D, Bircan I (2007). "Type 1 diabetes-related epidemiological, clinical and laboratory findings. An evaluation with special regard to autoimmunity in children". Saudi Med J. 28 (4): 584–9. PMID 17457482.
- ↑ Notkins, Abner Louis (2002). "Immunologic and Genetic Factors in Type 1 Diabetes". Journal of Biological Chemistry. 277 (46): 43545–43548. doi:10.1074/jbc.R200012200. ISSN 0021-9258.