Body mass index
|
WikiDoc Resources for Body mass index |
|
Articles |
|---|
|
Most recent articles on Body mass index Most cited articles on Body mass index |
|
Media |
|
Powerpoint slides on Body mass index |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Body mass index at Clinical Trials.gov Trial results on Body mass index Clinical Trials on Body mass index at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Body mass index NICE Guidance on Body mass index
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Body mass index Discussion groups on Body mass index Patient Handouts on Body mass index Directions to Hospitals Treating Body mass index Risk calculators and risk factors for Body mass index
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Body mass index |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Body mass index is a mathematic calculation that provides a measure for assessing the health risks associated with body weight. Numerous research studies confirm that body size below and particularly above a defined range increases the risk for health problems such as HEART DISEASE, as well as DIABETES and cancer.
The body mass index (BMI) provides a representation of body fat; the greater amount of body fat a person has, the higher the health risks. Health experts consider excess body weight from body fat the leading modifiable RISK FACTOR FOR HEART DISEASE.
The BMI Reference Chart gives whole value BMI figures by height and weight. Find height in inches in the left column, move across the row to closest weight, and read the BMI across the top row. For example, a person who is five-feet nine-inches tall is 69 inches. At a weight of 155 the BMI is 23. A person who is the same 69 inches tall but weighs 215 pounds has a BMI of about 32. Men and women of the same height and weight have the same BMI.
- A healthy BMI is 18.5 to 24.9. This reflects a ratio between weight and height that presents no
greater than the typical risks of health problems.
- A BMI below 18.5 reflects an increased risk of health problems associated with being underweight.
- A BMI from 25 to 29.9 reflects body weight that is 10-15% above what is healthy and double the risk for hypertension.
- A BMI over 30 reflects body weight that is 20% or more above healthy weight and 2-6 times the risk for cardiovascular disease of any kind.
- A BMI over 35 reflects nearly certain health problems related to obesity, most of which are cardiovascular such as hypertension, HYPERCHOLESTEROLEMIA or HYPERLIPIDEMIA, CORONARY ARTERY DISEASE, and HEART FAILURE.
Some people are in between the whole number BMI figures, are at the border between health risk classifications, or are not on the chart. In such situations, it is more effective to calculate the precise BMI by following these steps:

• Determine body weight in pounds (without clothing) • Measure height in inches • Multiply height in inches by itself (gives height in square inches) • Divide body weight in pounds by height in square inches • Multiply the answer by 703 • Result is BMI

BMI is one of numerous health indicators. People with BMIs in the “healthy weight” range can still have hypertension, coronary artery disease, and other cardiovascular conditions. Conversely, people with BMIs in ranges associated with increased risk for heart disease can have healthy cardiovascular systems.
BMI is not accurate for certain people—athletes with high muscle mass, pregnant women, people under age 18, and the very elderly. However, the correlation between BMI and cardiac health is strong. Body weight, or more appropriately body fat, is a modifiable risk factor.
To the extent possible, it is desirable for cardiovascular health (and health overall) to manage weight through nutrition, diet, and physical activity to maintain a BMI in the “healthy weight” range.
The BMI Tables:
Look up a patient's BMI in the table at this link:
http://www.nhlbi.nih.gov/guidelines/obesity/bmi_tbl.htm
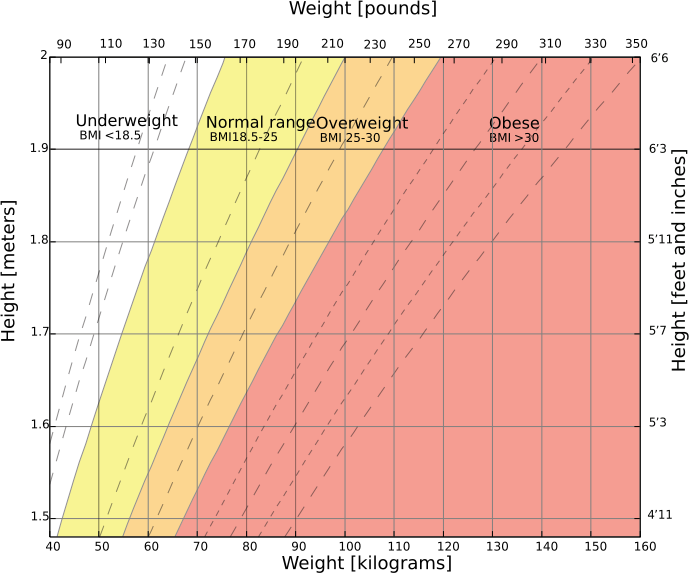
Based on World Health Organization data here.
Body mass index (BMI) or Quetelet Index is a statistical measure of the weight of a person scaled according to height. It was invented between 1830 and 1850 by the Belgian polymath Adolphe Quetelet during the course of developing "social physics".
Body mass index is defined as the individual's body weight divided by the square of their height. The formulas universally used in medicine produce a unit of measure of kg/m2. Body mass index may be accurately calculated using any of the formulas below.
| SI units | <math>\mathrm{BMI} = \frac{\mathit{weight} \ \mathrm{(kg)}}{\mathit{height}^2 (\mathrm{m^2})}</math> |
| US customary units | <math>\mathrm{BMI} = 703\times\frac{\mathit{weight} \ (\mathrm{lb})}{\mathit{height}^2 \ (\mathrm{in^2})}</math> |
| Imperial units | <math>\mathrm{BMI} = 6.35\times\frac{\mathit{weight} \ (\mathrm{stone})}{\mathit{height}^2 \ (\mathrm{m^2})}</math> |
BMI can also be determined using a BMI chart, which displays BMI as a function of weight (horizontal axis) and height (vertical axis) using contour lines for different values of BMI or colors for different BMI categories.
Usage
As a measure, BMI became popular during the early 1950s and 60s as obesity started to become a discernible issue in prosperous Western society. BMI provided a simple numeric measure of a person's "fatness" or "thinness", allowing health professionals to discuss over- and under-weight problems more objectively with their patients. However, BMI has become controversial because many people, including physicians, have come to rely on its apparent numerical authority for medical diagnosis, but that was never the BMI's purpose. It is meant to be used as a simple means of classifying sedentary (physically inactive) individuals with an average body composition.[1] For these individuals, the current value settings are as follows: a BMI of 18.5 to 25 may indicate optimal weight; a BMI lower than 18.5 suggests the person is underweight while a number above 25 may indicate the person is overweight; a BMI below 17.5 may indicate the person has anorexia or a related disorder; a number above 30 suggests the person is obese (over 40, morbidly obese).
For a given height the BMI is proportional to weight; for example, if body weight increases by 50%, BMI increases by 50%. For a given body shape and given density, the BMI is proportional to height--if all body dimensions increase by 50%, the BMI increases by 50%. This tendency for taller people to have higher BMIs is partially offset by the fact that many taller people are not just "scaled up" short people, but rather tend to have narrower frames in proportion to their height. [2]
BMI Prime
BMI Prime, a simple modification of the BMI system, is the ratio of actual BMI to upper limit BMI (currently defined at BMI 25). As defined, BMI Prime is also the ratio of body weight to upper body weight limit, calculated at BMI 25. Since it is the ratio of two separate BMI values, BMI Prime is a pure, dimensionless number, without associated units. Individuals with BMI Prime < 0.74 are underweight; those between 0.74 and 0.99 have optimal weight; and those at 1.00 or greater are overweight. BMI Prime is useful clinically because individuals can quantify, at a glance, what percentage they deviate from their upper weight limits. For instance, a person with BMI 34 has a BMI Prime of 34/25 = 1.36, and is 36% over his or her upper mass limit. In Asian populations (see International Variation section below) BMI Prime should be calculated using an upper limit BMI of 23 in the denominator instead of 25. Nonetheless, BMI Prime allows easy comparison between populations whose upper limit BMI values differ.[3]
Categories
A frequent use of the BMI is to assess how much an individual's body weight departs from what is normal or desirable for a person of his or her height. The weight excess or deficiency may, in part, be accounted for by body fat (adipose tissue) although other factors such as muscularity also affect BMI significantly (see discussion below and overweight). Human bodies rank along the index from around 15 (near starvation) to over 40 (morbidly obese). This statistical spread is usually described in broad categories: underweight, normal weight, overweight, obese and morbidly obese. The particular BMI values used to demarcate these categories varies based on the authority, the CDC[4] and the WHO[5] regard a BMI of less than 18.5 as underweight and may indicate malnutrition, an eating disorder, or other health problems, while a BMI greater than 25 is considered overweight and above 30 is considered obese. These ranges of BMI values are valid only as statistical categories when applied to adults, and do not predict health.
| Category | BMI range - kg/m2 | BMI Prime |
|---|---|---|
| Starvation | less than 15 | less than 0.60 |
| Underweight | from 15 to 18.5 | from 0.6 to 0.74 |
| Normal | from 18.5 to 25 | from 0.74 to 1.0 |
| Overweight | from 25 to 30 | from 1.0 to 1.2 |
| Obese | from 30 to 40 | from 1.2 to 1.6 |
| Morbidly Obese | greater than 40 | greater than 1.6 |
The U.S. National Health and Nutrition Examination Survey of 1994 indicates that 59% of American men and 49% of women have BMIs over 25. Extreme obesity — a BMI of 40 or more — was found in 2% of the men and 4% of the women. There are differing opinions on the threshold for being underweight in females, doctors quote anything from 18.5 to 20 as being the lowest weight, the most frequently stated being 19. A BMI nearing 15 is usually used as an indicator for starvation and the health risks involved, with a BMI <17.5 being an informal criterion for the diagnosis of anorexia nervosa.
BMI-for-age
BMI is used differently for children. It is calculated the same way as for adults, but then compared to typical values for other children of the same age. Instead of set thresholds for underweight and overweight, then, the BMI percentile allows comparison with children of the same sex and age.[6] A BMI that is less than the 5th percentile is considered underweight and above the 95th percentile is considered overweight. Children with a BMI between the 85th and 95th percentile are considered to be at risk of becoming overweight.
Recent studies in England have indicated that females between the ages 12 and 16 have a higher BMI than males by 1.0 kg/m² on average.[7]
International variations
These recommended distinctions along the linear scale may vary from time to time and country to country, making global, longitudinal surveys problematic. In 1998, the U.S. National Institutes of Health brought U.S. definitions into line with World Health Organization guidelines, lowering the normal/overweight cut-off from BMI 27.8 to BMI 25. This had the effect of redefining approximately 30 million Americans, previously "technically healthy" to "technically overweight". It also recommends lowering the normal/overweight threshold for South East Asian body types to around BMI 23, and expects further revisions to emerge from clinical studies of different body types.
In Singapore, the BMI cut-off figures were revised in 2005 with an emphasis on health risks instead of weight. Adults whose BMI is between 18.5 and 22.9 have a low risk of developing heart disease and other health problems such as diabetes. Those with a BMI between 23 and 27.4 are at moderate risk while those with a BMI of 27.5 and above are at high risk of heart disease and other health problems.[2]
These ranges of BMI values are valid only for Southeast Asian body type.
| Category | BMI range - kg/m2 |
|---|---|
| Starvation | less than 14.9 |
| Underweight | from 15 to 18.4 |
| Normal | from 18.5 to 22.9 |
| Overweight | from 23 to 27.5 |
| Obese | from 27.6 to 40 |
| Morbidly Obese | greater than 40 |
Applications
Statistical device
The Body Mass Index is generally used as a means of correlation between groups related by general mass and can serve as a vague means of estimating adiposity. The duality of the Body Mass Index is that, whilst easy-to-use as a general calculation, it is limited in how accurate and pertinent the data obtained from it can be. Generally, the Index is suitable for recognising trends within sedentary or overweight individuals because there is a smaller margin for errors.[8]
This general correlation is particularly useful for consensus data regarding obesity or various other conditions because it can be used to build a semi-accurate representation from which a solution can be stipulated, or the RDA for a group can be calculated. Similarly, this is becoming more and more pertinent to the growth of children, due to the majority of their exercise habits.[9]
The growth of children is usually documented against a BMI-measured growth chart. Obesity trends can be calculated from the difference between the child's BMI and the BMI on the chart. However, this method again falls prey to the obstacle of body composition: many children who are generally born, or grow as an endomorph, would be classed as obese despite body composition. Clinical professionals should take into account the child's body composition and defer to an appropriate technique such as densitometry.
Clinical practice
BMI has been used by the WHO as the standard for recording obesity statistics since the early 1980s. In the United States, BMI is also used as a measure of underweight, owing to advocacy on behalf of those suffering with eating disorders, such as anorexia nervosa and bulimia nervosa.
BMI can be calculated quickly and without expensive equipment. However, BMI categories do not take into account many factors such as frame size and muscularity.[10] The categories also fail to account for varying proportions of fat, bone, cartilage, water weight, and more. BMI is a statistical categorisation and therefore is not appropriate for diagnosing individuals.
Despite this, BMI categories are regularly regarded as a satisfactory tool for measuring whether sedentary individuals are "underweight," "overweight" or "obese" with various qualifications, such as: Individuals who are not sedentary being exempt - athletes, children, the elderly, the infirm, and individuals who are naturally endomorphic or ectomorphic (i.e., people who don't have a medium frame).
One basic problem, especially in athletes, is that muscle is denser than fat. Some professional athletes are "overweight" or "obese" according to their BMI - unless the number at which they are considered "overweight" or "obese" is adjusted upward in some modified version of the calculation. In children and the elderly, differences in bone density and, thus, in the proportion of bone to total weight can mean the number at which these people are considered underweight should be adjusted downward.
Methods for actually measuring body fat percentage are preferable to BMI for measuring body fat. Body fat has been statistically linked to some health problems and trends, but again, this is often a spurious relationship and there are no simple proofs of health based on such measurement.
Limitations and shortcomings
The medical establishment has generally acknowledged some shortcomings of BMI.[11] Because the BMI is dependent only upon net weight and height, it makes simplistic assumptions about distribution of muscle and bone mass, and thus may overestimate adiposity on those with more lean body mass (e.g. athletes) while underestimating adiposity on those with less lean body mass (e.g. the elderly).
In fact, some argue that the error in the BMI is significant and so pervasive that it is not generally useful in evaluation of health.[12] Due to these limitations, body composition for athletes is often better calculated using measures of body fat, as determined by such techniques as skinfold measurements or underwater weighing.
In an analysis of 40 studies involving 250,000 people, heart patients with normal BMIs were at higher risk of death from cardiovascular disease than people whose BMIs put them in the "overweight" range (BMI 25-29.9).[13] Patients who were underweight or severely overweight had an increased risk of death from cardiovascular disease. The implications of this finding can be confounded by the fact that many chronic diseases, such as diabetes, can cause weight loss before the eventual death. In light of this, higher death rates among thinner people would be the expected result.
BMI Calculator
http://www.nhlbisupport.com/bmi/bmicalc.htm
For Patients
Body mass index (BMI) is a measure of body fat based on height and weight that applies to both adult men and women.
- Enter your weight and height using Standard or Metric measures.
- Click on "Compute BMI" and your BMI will appear in the heart of the figure.
BMI Calculator: [[3]]
BMI Categories
- Underweight = <18.5
- Normal weight = 18.5-24.9
- Overweight = 25-29.9
- Obesity = BMI of 30 or greater
See also
- Waist-hip ratio
- Body fat percentage
- Muscle
- Skeletal muscle
- Basal metabolic rate
- Allometric law
References
- ↑ WHO Technical Report Series, #854, Physical Status: The Use and Interpretation of Anthropometry, Pg. 9 (2.1 MB PDF, here)
- ↑ Calculation of power law relationship between weight and height
- ↑ Gadzik J: "How Much Should I Weigh?" - Quetelet's Equation, Upper Weight Limits and BMI Prime Connecticut Medicine Feb 2006; 70: 81 - 88.
- ↑ About BMI for Adults
- ↑ BMI Classification
- ↑ BMI - Body Mass Index: BMI for Children and Teens
- ↑ Health Survey for England: The Health of Children and Young People
- ↑ Jeukendrup, A & Gleeson, M. (2005) Sports Nutrition Human Kinetics
- ↑ Barasi, M. E (2004) Human Nutrition - a health perspective
- ↑ Jeukendrup, A & Gleeson, M. (2005) Sports Nutrition Human Kinetics
- ↑ "Aim for a Healthy Weight: Assess your Risk". National Institutes of Health. 2007-07-08.
- ↑ "Is obesity such a big, fat threat?". Cox News Service. 2004-08-30. Retrieved 2007-07-08.
- ↑ "Association of bodyweight with total mortality and with cardiovascular events in coronary artery disease: a systematic review of cohort studies". Lancet. 2006-08-19;368(9536):666-78. Retrieved 2007-07-08. Check date values in:
|date=(help)